-
摘要: 目的 探讨嗅神经母细胞瘤的临床特点和经鼻内镜手术联合放/化疗的治疗效果。方法 回顾性分析2009年9月—2023年6月我院收治的接受经鼻内镜手术治疗的17例嗅神经母细胞瘤患者的临床、手术资料及随访结果。结果 17例患者中改良Kadish B期4例,C期10例,D期3例。10例患者一期行鼻内镜手术切除肿瘤(除外颈清),平均手术时长(5.2±2.5) h,平均出血量为(192.0±162.0) mL。15例患者行颅底重建,3例患者出现术后并发症,13例患者达到阴性切缘。所有患者均得以随访,平均随访(49.7±40.2)个月,死亡3例,复发和(或)转移6例。1、2和5年总体生存率分别为88.2%、80.2%和80.2%,1、2和5年无病生存率分别为82.4%、82.4%和50.8%。切缘阴性和切缘阳性的患者2年总体生存率分别为100.0%和25.0%,2年无病生存率分别为61.5%和25.0%。结论 经鼻内镜手术联合放/化疗治疗嗅神经母细胞瘤疗效可靠,切缘阳性患者预后较差。Abstract: Objective To investigate the clinical characteristics of esthesioneuroblastoma and the efficacy of endonasal endoscopic surgery combined with radiotherapy/chemotherapy.Methods The clinical and surgical data of 17 patients with esthesioneuroblastoma who underwent endonasal endoscopic surgery in our department from September 2009 to June 2023 were retrospectively analyzed.Results Among all patients, the modified Kadish stage B was identified in 4 patients, C in 10 patients, and D in 3 patients. Ten of them underwent endonasal endoscopic surgery without neck dissection in one day, whose average operation time is (5.2±2.5) hours and average blood loss is (192±162)mL. Skull base reconstructions were performed in 15 patients, postoperative complications were observed in 3 patients, and negative margins were obtained in 13 patients. All 17 patients were followed up for an average of (49.7±40.2) months. Three patients died and 6 had recurrence and/or metastasis. The 1-year, 2-year and 5-year overall survival rates were 88.2%, 80.2%, and 80.2%, respectively, and the 1-year, 2-year and 5-year disease-free survival rates were 82.4%, 82.4%, and 50.8%, respectively. The 2-year overall survival rates of patients with negative and positive margins were 100% and 25%, respectively, while the 2-year disease-free survival rates were 61.5% and 25.0%, respectively.Conclusion Endonasal endoscopic surgery combined with radiotherapy/chemotherapy can achieve satisfactory effect in esthesioneuroblastoma, and the prognosis of patients with positive margins is poor.
-
Key words:
- esthesioneuroblastoma /
- endonasal endoscope /
- surgical operation /
- prognosis
-

-
表 1 17例患者的临床特征、治疗方案和预后情况
例序 性别 年龄/岁 分期 颅底重建 并发症 切缘 Hyams分级 治疗方案 预后 1 男 61 C 鼻中隔黏膜瓣 脑脊液鼻漏 阴性 - 术前放疗+EES+颈清 存活 2 女 58 C 鼻中隔黏膜瓣 无 阴性 - EES,拒绝放疗 复发 3 女 55 C 人工脑膜+鼻中隔黏膜瓣 无 阴性 2 EES+放疗 复发 4 男 49 C 人工脑膜+鼻中隔黏膜瓣 无 阴性 2 EES+放疗 存活 5 男 39 B 人工脑膜+鼻中隔黏膜瓣 无 阴性 4 EES 复发 6 女 47 D 人工脑膜 无 阳性 4 分期EES+颈清+放疗+化疗 死亡 7 女 37 C 人工脑膜+鼻中隔黏膜瓣 复视、溢泪 阴性 3 EES+放疗 存活 8 男 32 B 人工脑膜+鼻中隔黏膜瓣 无 阴性 - EES 存活 9 男 59 C 人工脑膜+阔筋膜+颅周骨膜瓣 无 阳性 3 分期EES,拒绝放化疗 死亡 10 男 57 D 人工脑膜+鼻中隔黏膜瓣 无 阳性 - EES+颈清+放疗+化疗 死亡 11 男 48 C 鼻中隔黏膜瓣 无 阳性 2 诱导化疗+EES+放疗 存活 12 男 23 C 颅周骨膜瓣 休克、尿崩症 阴性 2 EES+放疗 存活 13 男 46 D 人工脑膜+阔筋膜+颅周骨膜瓣 无 阴性 3 EES+颈清+放疗+化疗 存活 14 男 47 C 鼻中隔黏膜瓣 无 阴性 - EES+放疗+化疗 存活 15 男 41 B 未行 无 阴性 1 EES 存活 16 女 41 B 未行 无 阴性 3 EES+放疗 存活 17 男 63 C 鼻中隔黏膜瓣 无 阴性 3 EES+放疗+化疗 存活 注:EES=endonasal endoscopic surgery,鼻内镜手术。 -
[1] Bak M, Wein RO. Esthesioneuroblastoma: a contemporary review of diagnosis and management[J]. Hematol Oncol Clin North Am, 2012, 26(6): 1185-1207. doi: 10.1016/j.hoc.2012.08.005
[2] Diaz EM Jr, Johnigan RH 3rd, Pero C, et al. Olfactory neuroblastoma: the 22-year experience at one comprehensive cancer center[J]. Head Neck, 2005, 27(2): 138-149. doi: 10.1002/hed.20127
[3] Fiani B, Quadri SA, Cathel A, et al. Esthesioneuroblastoma: A Comprehensive Review of Diagnosis, Management, and Current Treatment Options[J]. World Neurosurg, 2019, 126: 194-211. doi: 10.1016/j.wneu.2019.03.014
[4] Morita A, Ebersold MJ, Olsen KD, et al. Esthesioneuroblastoma: prognosis and management[J]. Neurosurgery, 1993, 32(5): 706-714. doi: 10.1227/00006123-199305000-00002
[5] Malouf GG, Casiraghi O, Deutsch E, et al. Low-and high-grade esthesioneuroblastomas display a distinct natural history and outcome[J]. Eur J Cancer, 2013, 49(6): 1324-1334. doi: 10.1016/j.ejca.2012.12.008
[6] 贺新娣, 王英. 31例嗅神经母细胞瘤临床分析[J]. 临床耳鼻咽喉头颈外科杂志, 2021, 35(4): 338-340. doi: 10.13201/j.issn.2096-7993.2021.04.012
[7] Tosoni A, Di Nunno V, Gatto L, et al. Olfactory neuroblastoma: diagnosis, management, and current treatment options[J]. Front Oncol, 2023, 13: 1242453. doi: 10.3389/fonc.2023.1242453
[8] Shahangian A, Soler ZM, Baker A, et al. Successful repair of intraoperative cerebrospinal fluid leaks improves outcomes in endoscopic skull base surgery[J]. Int Forum Allergy Rhinol, 2017, 7(1): 80-86. doi: 10.1002/alr.21845
[9] Roxbury CR, Ishii M, Gallia GL, et al. Endoscopic Management of Esthesioneuroblastoma[J]. Otolaryngologic Clinics of North America, 2016, 49(1): 153-165. doi: 10.1016/j.otc.2015.09.010
[10] Spielman DB, Liebowitz A, Grewal M, et al. Exclusively endoscopic surgical resection of esthesioneuroblastoma: A systematic review[J]. World J Otorhinolaryngol Head Neck Surg, 2022, 8(1): 66-72. doi: 10.1002/wjo2.10
[11] 孙炎, 黄谦, 崔顺九, 等. Kadish C期嗅神经母细胞瘤行鼻内镜手术切除及综合治疗的临床分析[J]. 中国耳鼻咽喉颅底外科杂志, 2020, 26(2): 114-120. https://www.cnki.com.cn/Article/CJFDTOTAL-ZEBY202002002.htm
[12] Duo GS, Feng JL, Zhang ZY, et al. Survival impact of postoperative radiotherapy in patients with olfactory neuroblastoma: 513 cases from the SEER database[J]. Cancer Radiother, 2022, 26(5): 663-669. doi: 10.1016/j.canrad.2021.12.006
[13] Lechner M, Takahashi Y, Turri-Zanoni M, et al. Clinical outcomes, Kadish-INSICA staging and therapeutic targeting of somatostatin receptor 2 in olfactory neuroblastoma[J]. Eur J Cancer, 2022, 162: 221-236. doi: 10.1016/j.ejca.2021.09.046
-

| 引用本文: | 顾月龙, 茆松, 唐如, 等. 经鼻内镜手术治疗嗅神经母细胞瘤的临床分析[J]. 临床耳鼻咽喉头颈外科杂志, 2024, 38(6): 503-507. doi: 10.13201/j.issn.2096-7993.2024.06.009 |
| Citation: | GU Yuelong, MAO Song, TANG Ru, et al. Clinical analysis of endonasal endoscopic surgery in esthesioneuroblastoma[J]. J Clin Otorhinolaryngol Head Neck Surg, 2024, 38(6): 503-507. doi: 10.13201/j.issn.2096-7993.2024.06.009 |
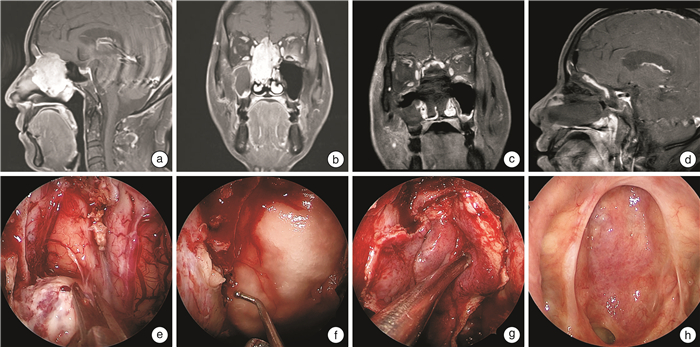
- Figure 1.
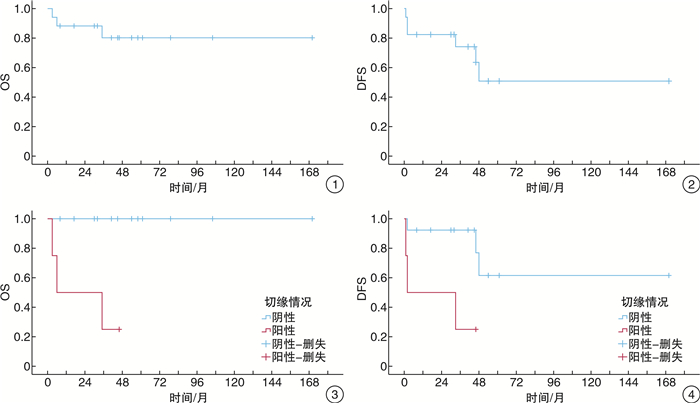
- Figure 5.



 下载:
下载: