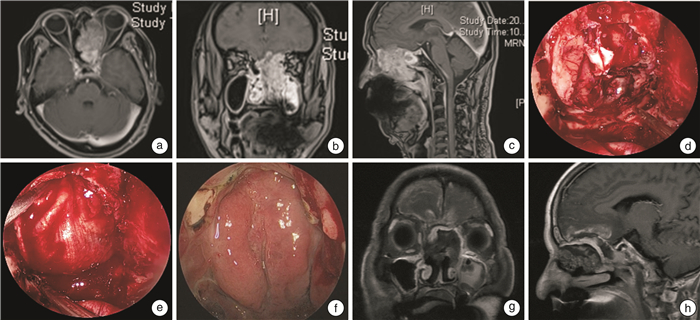
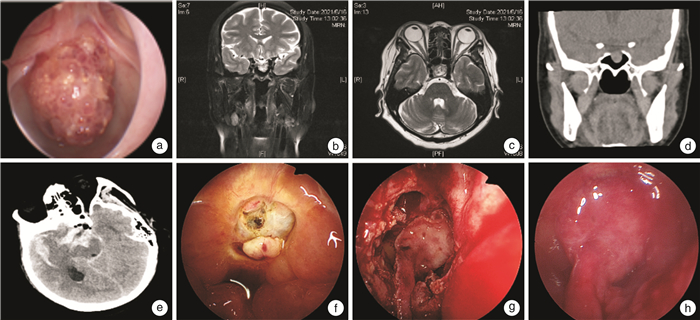
Clinical analysis of resection and dura skull base reconstruction of cranionasal communication tumor in 31 cases
-
摘要: 目的 探讨颅鼻沟通瘤切除与硬脑膜颅底修复重建方法。方法 收集2018-2022年接受颅鼻沟通瘤切除术后行硬脑膜颅底重建的31例患者的临床资料,并随访3~41个月。结果 总计31例患者,其中男20例,女11例;年龄19~74岁,中位年龄57岁。良性病变17例(血管瘤、Rathke囊肿、鳞状上皮乳头状瘤、颅咽管瘤各1例,脑膜脑膨出、内翻性乳头状瘤、脑膜瘤Ⅰ级各2例,神经鞘瘤3例,垂体瘤4例),恶性病变14例(骨肉瘤、低分化癌各1例,内翻性乳头状瘤恶变、嗅神经母细胞瘤、腺癌、腺样囊性癌各2例,鳞癌4例)。鼻内镜联合颅面切口16例,单纯鼻内镜手术15例。31例患者均行肿物手术全切及硬脑膜颅底重建,游离组织修复8例(阔筋膜5例,鼻腔黏膜3例);带蒂皮瓣修复23例(单纯鼻中隔黏膜瓣11例,鼻中隔黏膜瓣联合游离移植物6例,帽状腱膜联合游离移植物6例);31例患者中有8例行颅底骨性修复。术后脑出血1例,脑脊液漏1例,颅内感染2例,治疗后均顺利出院。放疗后脑脊液漏伴颅内感染1例,保守治疗康复。17例良性病变患者均生存;14例恶性患者术后13例行放疗,9例无复发生存;5例复发,其中2例带瘤生存,1例再次手术,2例死亡。结论 颅鼻沟通瘤是前中颅底的高危疾病,肿物完整切除后修复方式多种多样,良好的修复重建及多学科协作对患者的预后至关重要。Abstract: Objective To explore the methods of resection, dura and skull base repair and reconstruction of cranionasal communication tumor.Methods Data of 31 patients with cranionasal communication tumor who underwent dura and skull base reconstruction after tumor resection from 2018 to 2022 were collected. Follow-up lasted for 3 to 41 months.Results A total of 31 patients were enrolled, including 20 males and 11 females. The ages ranged from 19 to 74 years, with a median age of 57 years old. There were 17 benign lesions(one case of hemangioma, one case of Rathke cyst, one case of squamous papilloma, one case of craniopharyngioma, two cases of meningocele, two cases of varus papilloma, two cases of meningioma of grade Ⅰ, three cases of schwannoma, four cases of pituitary tumor) and 14 malignant lesions(one case of osteosarcoma, one case of poorly differentiated carcinoma, two cases of varus papilloma malignancy, two cases of olfactory neuroblastoma, two cases of adenocarcinoma, two cases of adenoid cystic carcinoma, four cases of squamous cell carcinoma). Sixteen cases underwent nasal endoscopy combined with craniofacial incision and 15 cases underwent nasal endoscopy surgery alone. Complete resection of the mass and dura and skull base reconstruction were performed in all 31 patients, and free graft repair was performed in 8 cases(fascia lata in 5 cases and nasal mucosa in 3 cases). Twenty-three cases were repaired with pedicled flaps(septal mucosal flap alone in 11 cases, septal mucosal flap combined with free graft in 6 cases, and cap aponeurosis combined with free graft in 6 cases). Eight out of 31 patients underwent skull base bone repair. Postoperative cerebral hemorrhage occurred in 1 case, cerebrospinal fluid leakage in 1 case, intracranial infection in 2 cases. All patients were successfully treated without severe sequelae. Cerebrospinal fluid leakage and intracranial infection occurred in one patient after radiotherapy, who recovered after conservative treatment. All 17 patients with benign lesions survived. Thirteen out of 14 patients with malignant lesions received radiotherapy after surgery, nine survived without recurrence, five cases recurred, of which 2 survived with tumor, one underwent reoperation and 2 died.Conclusion Cranionasal communication tumors are high-risk diseases of anterior and middle skull base, and various surgical repair methods could be selected after complete resection of the tumor. Successful reconstruction and multidisciplinary cooperation are crucial for treatment outcome.
-

-
[1] 王德辉, 孙希才. 内镜颅底外科团队: 未来颅底疾病治疗的主力军[J]. 中华耳鼻咽喉头颈外科杂志, 2021, 56(1): 3-6.
[2] 伊志强, 鲍圣德, 李良, 等. 多学科合作切除颅底沟通性肿瘤[J]. 中华神经外科杂志, 2012, 28(8): 768-771. doi: 10.3760/cma.j.issn.1001-2346.2012.08.007
[3] 董浩, 李永, 邱锷, 等. 鼻内镜联合显微外科手术治疗前中颅底沟通性肿瘤的手术疗效分析(附38例报告)[J]. 中华神经外科杂志, 2020, 36(7): 722-725. doi: 10.3760/cma.j.cn112050-20190418-00160
[4] 张强, 施铭岗, 刘钢, 等. 内镜经鼻联合显微镜额眶颧颞入路处理颅内外沟通性肿瘤的临床分析[J]. 中华耳鼻咽喉头颈外科杂志, 2021, 56(1): 33-40. doi: 10.3760/cma.j.cn115330-20200803-00645
[5] 时光刚, 何明强, 李秀国, 等. 额眶筛入路切除前中颅底颅鼻眶沟通瘤[J]. 中华耳鼻咽喉头颈外科杂志, 2005, 40(7): 521-523. doi: 10.3760/j.issn:1673-0860.2005.07.011
[6] 陈政源, 寿雪飞, 沈明, 等. 神经内镜经鼻入路切除颅底肿瘤术中颅底重建的临床疗效[J]. 中华神经外科杂志, 2020, 36(1): 2-6. doi: 10.3760/cma.j.issn.1001-2346.2020.01.002
[7] 王振霖, 张秋航, 郭宏川, 等. 单纯内镜经鼻入路切除前颅底颅内外沟通脑膜瘤的早期经验[J]. 中华耳鼻咽喉头颈外科杂志, 2013, 48(10): 807-813. doi: 10.3760/cma.j.issn.1673-0860.2013.10.004
[8] 刘全, 王欢, 孙希才, 等. 内镜经鼻入路切除前颅底恶性肿瘤的疗效观察[J]. 中华耳鼻咽喉头颈外科杂志, 2021, 56(1): 11-17.
[9] Bhatki AM, Carrau RL, Snyderman CH, et al. Endonasal surgery of the ventral skull base-endoscopic transcranial surgery[J]. Oral Maxillofac Surg Clin North Am, 2010, 22(1): 157-168. doi: 10.1016/j.coms.2009.10.005
[10] 张维天, 殷善开. 内镜下带血管蒂鼻中隔黏骨膜瓣修复颅底缺损[J]. 中华耳鼻咽喉头颈外科杂志, 2011, 46(6): 463-468. doi: 10.3760/cma.j.issn.1673-0860.2011.06.006
[11] Gil Z, Margalit N. Anteriorly based inferior turbinate flap for endoscopic skull base reconstruction[J]. Otolaryngol Head Neck Surg, 2012, 146(5): 842-847. doi: 10.1177/0194599811434516
[12] Yip J, Macdonald KI, Lee J, et al. The inferior turbinate flap in skull base reconstruction[J]. J Otolaryngol Head Neck Surg, 2013, 42(1): 6. doi: 10.1186/1916-0216-42-6
[13] DE Andrade EJ, Almeida JP, Borghei-Razavi H, et al. Reconstruction after extended endonasal approaches to the anterior cranial base: surgical techniques and current results[J]. J Neurosurg Sci, 2021, 65(2): 151-159.
[14] Gutierrez WR, Bennion DM, Walsh JE, et al. Vascular pedicled flaps for skull base defect reconstruction[J]. Laryngoscope Investig Otolaryngol, 2020, 5(6): 1029-1038. doi: 10.1002/lio2.471
[15] Clavenna MJ, Turner JH, Chandra RK. Pedicled flaps in endoscopic skull base reconstruction: review of current techniques[J]. Curr Opin Otolaryngol Head Neck Surg, 2015, 23(1): 71-77. doi: 10.1097/MOO.0000000000000115
[16] Lal D, Cain RB. Updates in reconstruction of skull base defects[J]. Curr Opin Otolaryngol Head Neck Surg, 2014, 22(5): 419-428. doi: 10.1097/MOO.0000000000000082
[17] Hadad G, Bassagasteguy L, Carrau RL, et al. A novel reconstructive technique after endoscopic expanded endonasal approaches: vascular pedicle nasoseptal flap[J]. Laryngoscope, 2006, 116(10): 1882-1886. doi: 10.1097/01.mlg.0000234933.37779.e4
[18] Eloy JA, Marchiano E, Vázquez A, et al. Management of Skull Base Defects After Surgical Resection of Sinonasal and Ventral Skull Base Malignancies[J]. Otolaryngol Clin North Am, 2017, 50(2): 397-417. doi: 10.1016/j.otc.2016.12.013
[19] Bassett E, Farag A, Iloreta A, et al. The extended nasoseptal flap for coverage of large cranial base defects[J]. Int Forum Allergy Rhinol, 2016, 6(11): 1113-1116. doi: 10.1002/alr.21778
[20] Tomio R, Toda M, Tomita T, et al. Primary dural closure and anterior cranial base reconstruction using pericranial and nasoseptal multi-layered flaps in endoscopic-assisted skull base surgery[J]. Acta Neurochir(Wien), 2014, 156(10): 1911-1915.
[21] Nyquist GG, Anand VK, Singh A, et al. Janus flap: bilateral nasoseptal flaps for anterior skull base reconstruction[J]. Otolaryngol Head Neck Surg, 2010, 142(3): 327-331.
[22] Bozkurt G, Leone F, Arosio AD, et al. Septal Flip Flap for Anterior Skull Base Reconstruction After Endoscopic Transnasal Craniectomy: Long-Term Outcomes[J]. World Neurosurg, 2019, 128: e409-e416.
[23] Mao S, Li M, Li D, et al. Septal floor rotational flap pedicled on ethmoidal arteries for endoscopic skull base reconstruction[J]. Laryngoscope, 2019, 129(12): 2696-2701.
[24] Soyka MB, Serra C, Regli L, et al. Long-term olfactory outcome after nasoseptal flap reconstructions in midline skull base surgery[J]. Am J Rhinol Allergy, 2017, 31(5): 334-337.
[25] Lavigne P, Faden DL, Wang EW, et al. Complications of Nasoseptal Flap Reconstruction: A Systematic Review[J]. J Neurol Surg B Skull Base, 2018, 79(Suppl 4): S291-S299.
[26] Hanson M, Patel PM, Betz C, et al. Sinonasal outcomes following endoscopic anterior skull base surgery with nasoseptal flap reconstruction: a prospective study[J]. J Laryngol Otol, 2015, 129 Suppl 3: S41-46.
[27] Patel MR, Shah RN, Snyderman CH, et al. Pericranial flap for endoscopic anterior skull-base reconstruction: clinical outcomes and radioanatomic analysis of preoperative planning[J]. Neurosurgery, 2010, 66(3): 506-512.
[28] García-Fernández A, García-González E, Paredes-Sansinenea I, et al. Hidden Port Approach to Endoscopic Pericranial Scalp Flap for Anterior Skull Base Reconstruction[J]. Laryngoscope, 2021, 131(8): 1749-1752.
[29] Gabriel PJ, Kohli G, Hsueh WD, et al. Efficacy of simultaneous pericranial and nasoseptal "double flap" reconstruction of anterior skull base defects after combined transbasal and endoscopic endonasal approaches[J]. Acta Neurochir(Wien), 2020, 162(3): 641-647.
[30] McCoul ED, Anand VK, Singh A, et al. Long-term effectiveness of a reconstructive protocol using the nasoseptal flap after endoscopic skull base surgery[J]. World Neurosurg, 2014, 81(1): 136-143.
[31] Horiguchi K, Nishioka H, Fukuhara N, et al. A new multilayer reconstruction using nasal septal flap combined with fascia graft dural suturing for high-flow cerebrospinal fluid leak after endoscopic endonasal surgery[J]. Neurosurg Rev, 2016, 39(3): 419-427.
[32] Eloy JA, Patel SK, Shukla PA, et al. Triple-layer reconstruction technique for large cribriform defects after endoscopic endonasal resection of anterior skull base tumors[J]. Int Forum Allergy Rhinol, 2013, 3(3): 204-211.
[33] 邓跃飞, 刘正豪, 郑眉光, 等. 帽状腱膜下层骨膜瓣和钛板联合修复前颅底沟通肿瘤术后颅底巨大骨缺损的疗效观察[J]. 中华神经外科杂志, 2015, 31(2): 155-157.
[34] 张秋航, 严波, 李长青, 等. 内镜经鼻入路前颅底重建[J]. 中华耳鼻咽喉头颈外科杂志, 2007, 42(5): 324-327. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHEB200705002.htm
[35] Tang IP, Carrau RL, Otto BA, et al. Technical nuances of commonly used vascularised flaps for skull base reconstruction[J]. J Laryngol Otol, 2015, 129(8): 752-761.
[36] Hachem RA, Elkhatib A, Beer-Furlan A, et al. Reconstructive techniques in skull base surgery after resection of malignant lesions: a wide array of choices[J]. Curr Opin Otolaryngol Head Neck Surg, 2016, 24(2): 91-97.
[37] Kassam AB, Thomas A, Carrau RL, et al. Endoscopic reconstruction of the cranial base using a pedicled nasoseptal flap[J]. Neurosurgery, 2008, 63(1 Suppl 1): ONS44-52.
-




 下载:
下载: