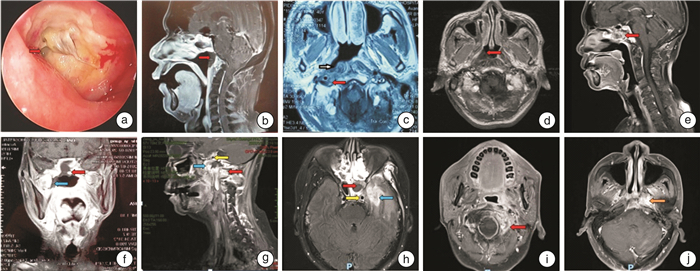
Clinical classification, staging and treatment strategy of radionecrosis of the nasopharynx and skull base
-
摘要: 目的 本研究旨在通过对鼻咽癌放疗后的放射性颅底坏死病例的回顾性分析,探讨建立一种用于指导临床治疗和预后风险评估的分型分期系统。方法 总结广西壮族自治区人民医院耳鼻咽喉头颈外科2019年1月—2022年12月共计86例放射性颅底坏死患者的临床资料,其中17例放弃治疗,69例进行治疗。通过分析69例患者的电子鼻咽喉镜检查结合MRI、CT等影像学检查,提出放射性颅底坏死分型分期系统,进一步分析分型分期系统与患者的手术情况、手术效果和预后的关系。结果 根据放射性颅底坏死对软组织、骨质、重要血管神经的破坏程度及范围,将其分为闭合型(5例)和开放型(64例),其中开放型又分5型:Ⅰ型(4例),Ⅱ型(6例),Ⅲ型(39例,其中Ⅲa型21例,Ⅲb型18例),Ⅳ型(12例),Ⅴ型(8例)。根据鼻内镜检查联合MRI或CT等影像学检查,结合是否二程放疗、感染累及的部位、骨质破坏范围、颈内动脉累犯程度、脑组织坏死程度进行计分和统计,按不同分数级别将病变分为4期:Ⅰ期4例(1~2分),Ⅱ期11例(3~4分),Ⅲ期24例(5~6分),Ⅳ期30例(≥7分)。69例患者中,22例选择保守治疗:Ⅰ期2例,Ⅱ期3例,Ⅲ期7例,Ⅳ期10例;47例选择鼻内镜手术治疗:Ⅰ期2例、Ⅱ期8例、Ⅲ期17例、Ⅳ期20例,其中16例行游离黏膜瓣和(或)带蒂鼻中隔黏膜瓣鼻咽颅底修复。按分期划分,Ⅰ、Ⅱ、Ⅲ期患者手术治疗后均获得较好效果,分期越高的患者预后越差,且围手术期并发症发生率越高。术后并发症有手术部位感染无法愈合、脑脊液鼻漏、进展性骨坏死、鼻咽部大出血及死亡等。结论 放射性颅底坏死的分型分期系统可在定期随访中早期发现病变,在发现病变后能更好地应用于临床治疗指导和风险预后评估。Abstract: Objective To establish a staging system for guiding clinical treatment and prognostic risk assessment by retrospectively analyzing the cases with radionecrosis of the nasopharynx and skull base (RNSB) after radiotherapy for nasopharyngeal carcinoma.Methods A total of 86 cases of RNSB from January 2019 to December 2022 visited Department of Otorhinolaryngology Head and Neck, the People's Hospital of Guangxi Zhuang Autonomous Region. Seventeen patients gave up the treatment, and 69 patients who underwent treatment were included for analysis. By analyzing the results of electronic nasopharyngolaryngoscopy combined with magnetic resonance (MR), CT, and other imaging examinations, a staging system for RNSB was proposed. The relationship between the staging system and the surgical effectiveness and clinical prognosis was further analyzed.Results According to the severity and extent of destruction of soft tissue, bone, and the adjacent neurovascular structures, the RNSB was categorized into closed type (n=5) and open type (n=64), of which the open type was subdivided into five types: type Ⅰ(n=4), type Ⅱ(n=6), type Ⅲ(n=39, of which 21 cases were type Ⅲa and 18 cases were type Ⅲb), type Ⅳ(n=12), and type Ⅴ(n=8). The clinical stage of RNSB were classified based on nasopharyngolaryngoscopy and imaging examinations, receiving the second course of radiotherapy or not, the involvement of the infection site, the extent of bone destruction, the degree of internal carotid artery involvement, and the degree of brain tissue necrosis: stageⅠ(1-2 scores), 11 cases at stageⅡ(3-4 scores), 24 cases at stage Ⅲ(5-6 scores), and 30 cases at stage Ⅳ(≥ 7 scores or more). Twenty-two patients chose conservative treatment (2 patients at stage Ⅰ, 3 patients at stage Ⅱ, 7 patients at stage Ⅲ, and 10 patients at stage Ⅳ). Forty-seven patients chose nasal endoscopic surgical treatment (2 patients at stage Ⅰ, 8 patients at stage Ⅱ, 17 patients at stage Ⅲ, and 20 patients at stage Ⅳ), of which 16 cases had received free mucosal flap and/or stented septum mucosal flap repair. Patients at stages Ⅰ, Ⅱ, and Ⅲ achieved satisfactory efficacy after surgical treatment. In addition, higher clinical stage was found to correlate with the worse prognosis and higher incidence of perioperative complications, which included failure of healing because of surgical site infection, cerebrospinal fluid nasal leakage, progressive osteonecrosis, nasopharyngeal hemorrhage, and death.Conclusion The staging system proposed in our study can be used for early detection of RNSB during regular follow-up, and is also valuable for clinical treatment guidance and prognosis assessment.
-

-
表 1 放射性鼻咽颅底骨坏死分期分数计分方案
累犯病变范围 计分项目 分数 二程放疗(R) 否 0 是 1 感染累及部位(I) 无感染症状和体征 0 鼻咽腔软组织、头长肌 1 咽旁间隙、咽鼓管区、翼腭窝 2 颞下窝、颈静脉孔区、椎旁软组织 3 骨质破坏范围(E) 无骨质破坏 0 上颌骨、筛骨骨质破坏 1 枕骨斜坡、蝶窦骨质破坏 2 岩骨、颈椎骨质破坏 3 颈内动脉累犯程度(V) 与颈内动脉内侧缘距离>5 mm 0 与颈内动脉内侧缘距离<5 mm,或紧贴颈内动脉内侧缘 1 病变累及颈内动脉,颈内动脉壁包绕范围<1/2 2 病变累及颈内动脉,颈内动脉壁包绕范围>1/2,或将颈内动脉全包绕 3 脑组织坏死情况(N) 无硬脑膜及脑组织坏死 0 累及局部硬脑膜坏死 1 合并脑组织坏死 2 脑干受压变形 3 表 2 非手术治疗患者的临床疗效观察
例 分期 治愈 稳定 进展 死亡 P Ⅰ期 2 0 0 0 0.0142 Ⅱ期 2 1 0 0 Ⅲ期 0 4 1 2* Ⅳ期 0 4 2 4 *代表非手术治疗的Ⅲ期死亡患者中有1例死于远处转移。 表 3 鼻内镜手术治疗患者的临床疗效观察
例 分期 治愈 稳定 进展 死亡 P Ⅰ期 2 0 0 0 <0.012 Ⅱ期 7 1 0 0 Ⅲ期 9 5 1 2 Ⅳ期 0 5 1 14* *代表手术治疗的Ⅳ期死亡患者中有5例分别死于远处转移及新冠肺炎。 表 4 69例患者基线资料比较
例(%),X±S 因素 非手术组(n=22) 手术组(n=47) P 年龄/岁 53.5±10.0 53.4±9.10 0.977 性别 0.101 男 19(86.4) 30(63.8) 女 3(13.6) 17(36.2) 二程放疗 16(72.7) 39(83.0) 0.349 -
[1] 章华, 高可雷, 谢志海, 等. 内镜手术治疗鼻咽癌放射治疗后颅底软组织坏死的临床研究[J]. 中华耳鼻咽喉头颈外科杂志, 2021, 56(1): 26-32.
[2] 汤轶强, 敖帆, 黄敏, 等. 放射性鼻咽颅底骨坏死的S-B分期探讨[J]. 实用癌症杂志, 2020, 35(4): 561-563. doi: 10.3969/j.issn.1001-5930.2020.04.011
[3] 邱前辉, 陈海铃, 崔毅, 等. 鼻咽癌放疗后颅底组织坏死的CT影像分级及手术治疗探讨[J]. 中国临床新医学, 2023, 16(1): 1-7. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYLN202301001.htm
[4] Sathasivam HP, Davies GR, Boyd NM. Predictive factors for osteoradionecrosis of the jaws: A retrospective study[J]. Head Neck, 2018, 40(1): 46-54. doi: 10.1002/hed.24907
[5] Spillinger A, Park K, Shenouda K, et al. Endoscopic management of postradiation skull base osteoradionecrosis[J]. Int Forum Allergy Rhinol, 2020, 10(12): 1329-1333. doi: 10.1002/alr.22715
[6] 兰桂萍, 黄波, 司勇锋, 等. 内镜经鼻入路处理鼻咽癌放疗后颅底骨坏死临床体会[J]. 中华耳鼻咽喉头颈外科杂志, 2016, 51(5): 367-371. doi: 10.3760/cma.j.issn.1673-0860.2016.05.010
[7] Komune N, Matsuo S, Miki K, et al. Surgical Anatomy of the Eustachian Tube for Endoscopic Transnasal Skull Base Surgery: A Cadaveric and Radiologic Study[J]. World Neurosurg, 2018, 112: e172-e181. doi: 10.1016/j.wneu.2018.01.003
[8] Wang WH, Lieber S, Mathias RN, et al. The foramen lacerum: surgical anatomy and relevance for endoscopic endonasal approaches[J]. J Neurosurg, 2018: 1-12.
[9] 李峰, 蔡泽虹, 许卫华, 等. 鼻黏膜瓣在鼻咽癌放疗后鼻咽颅底骨质裸露修复中的应用[J]. 临床耳鼻咽喉头颈外科杂志, 2021, 35(10): 929-934. 10.13201/j.issn.2096-7993.2021.10.014
[10] 高俊潇, 邱前辉. 黏膜瓣在鼻咽癌放疗后鼻内镜手术修复颅底组织缺损中的应用[J]. 山东大学耳鼻喉眼学报, 2019, 33(2): 46-50. https://www.cnki.com.cn/Article/CJFDTOTAL-SDYU201902009.htm
[11] 邹雄, 王顺兰, 刘友平, 等. 经鼻内镜鼻咽坏死清创联合带血管蒂鼻腔黏骨膜瓣修复术治疗鼻咽癌放疗后鼻咽坏死[J]. 癌症, 2020, 39(6): 271-282. https://www.cnki.com.cn/Article/CJFDTOTAL-AIZH202006004.htm
[12] 高可雷, 章华, 谢志海, 等. 颞肌瓣在鼻咽癌放疗后肿瘤或坏死灶切除术后修复重建中的应用[J]. 中华耳鼻咽喉头颈外科杂志, 2022, 57(11): 1288-1293.
[13] Adel M, Chang KP. Using a nasoseptal flap for the reconstruction of osteoradionecrosis in nasopharyngeal carcinoma: a case report[J]. J Otolaryngol Head Neck Surg, 2016, 45: 27.
[14] Vlantis AC, Wong E, Chiu TW, et al. Vastus Lateralis Muscle Free Flap for Skull Base Osteoradionecrosis in Nasopharyngeal Carcinoma[J]. J Neurol Surg B Skull Base, 2018, 79(4): 349-352.
-




 下载:
下载: