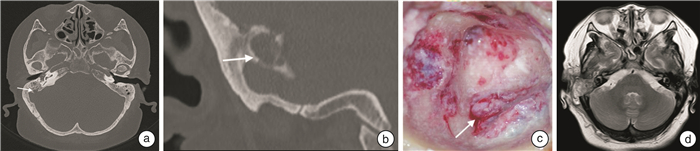
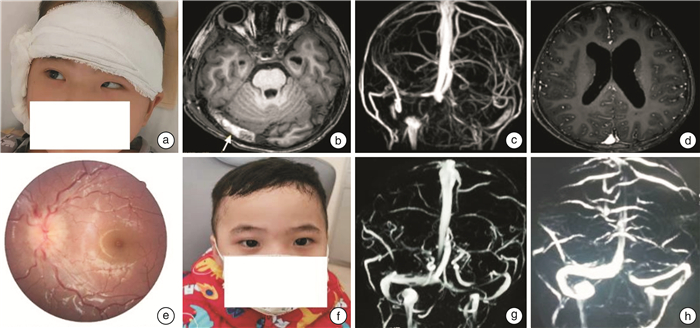
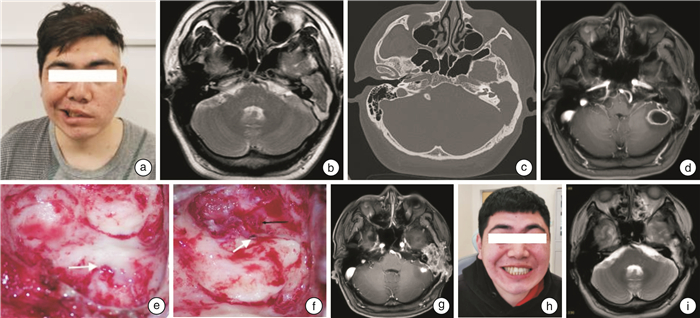
Clinical analysis of 11 cases of otogenic intracranial complications treated by multidisciplinary collaboration
-
摘要: 目的 分析耳源性颅内并发症的临床诊断、治疗方式及手术时机的选择。方法 收集2014年12月—2022年6月就诊于山东大学齐鲁医院(青岛)耳鼻咽喉头颈外科以耳部症状为首发表现的颅内并发症共11例患者的临床资料,其中男8例,女3例,年龄4~69岁。所有患者均有完善的耳内镜检查、听力学检查、影像学检查及病原学检查。采取神经内科、神经外科、感染科、影像科及耳鼻咽喉科多学科协作模式,根据临床症状危急程度、影像学变化情况,共同制定抗感染药物治疗及手术治疗方案。11例患者中,有5例神经外科先处理颅内病变,耳鼻咽喉科后处理中耳病变;3例脑膜炎患者先控制急性期脑炎症状,后处理中耳病变,1例中耳病变和颅内感染灶同期处理,2例处理中耳病变后,乙状窦、横窦血栓行保守治疗。随访时间为1~6年。采用描述性统计学方法进行分析。结果 11例患者均有时间不等的耳部症状,表现为耳痛、流脓、听力下降等,后出现发烧、头痛、意识障碍、面瘫等颅内并发症表现。耳内镜检查表现为鼓膜松弛部穿孔5例、紧张部大穿孔3例,耳道新生物1例,鼓膜膨出1例,鼓膜浑浊内陷1例。听力学检查传导性听力下降4例,混合性听力下降4例,全聋3例。影像学检查提示中耳胆脂瘤合并颞叶脑脓肿4例、小脑脓肿2例,中耳胆脂瘤合并脑膜炎3例,中耳感染合并乙状窦血栓性静脉炎2例。病原学检查中,脑脓肿脓液及脑脊液培养肺炎链球菌2例次,前庭链球菌、单形拟杆菌、奇异变形杆菌各1例次。随访过程中,1例出院后3年因合并心血管疾病去世,其余10例健在,定期复查颅内及中耳病变无复发。结论 耳源性颅内并发症以脑脓肿、脑膜炎及乙状窦血栓性静脉炎最常见,中耳胆脂瘤为最常见的病因。及时诊断、多学科协作、原发灶及合并症处理时机的准确把握提高了本病的治愈率。Abstract: Objective To analyze the clinical diagnosis, treatment, and surgical timing of otogenic intracranial complications.Methods The clinical data of 11 patients with intracranial complications with ear symptoms as the first manifestation in Department of Otorhinolaryngology Head and Neck Surgery, Qilu Hospital of Shandong University(Qingdao) from December 2014 to June 2022 were collected, including 8 males and 3 females, aged from 4 to 69 years. All patients had complete otoendoscopy, audiology, imaging and etiology examination, and the diagnosis and treatment plan was jointly developed through multidisciplinary consultation according to the critical degree of clinical symptoms and imaging changes. Among the 11 patients, 5 cases were treated with intracranial lesions first in neurosurgery department and middle ear lesions later in otolaryngology, 3 cases of meningitis, were treated with middle ear surgery after intracranial infection control, 1 case was treated with middle ear lesions and intracranial infection simultaneously, and 2 cases were treated with sigmoid sinus and transverse sinus thrombosis conservatively. They were followed up for 1-6 years. Descriptive statistical methods were used for analysis.Results All the 11 patients had ear varying symptoms, including ear pain, pus discharge and hearing loss, etc, and then fever appeared, headache, disturbance of consciousness, facial paralysis and other intracranial complication. Otoendoscopy showed perforation of the relaxation of the tympanic membrane in 5 cases, major perforation of the tension in 3 cases, neoplasia in the ear canal in 1 case, bulging of the tympanic membrane in 1 case, and turbidity of the tympanic membrane in 1 case. There were 4 cases of conductive hearing loss, 4 cases of mixed hearing loss and 3 cases of total deafness. Imaging examination showed cholesteatoma of the middle ear complicated with temporal lobe brain abscess in 4 cases, cerebellar abscess in 2 cases, cholesteatoma of the middle ear complicated with intracranial infection in 3 cases, and sigmoid sinus thrombophlebitis in 2 cases. In the etiological examination, 2 cases of Streptococcus pneumoniae were cultured in the pus of brain abscess and cerebrospinal fluid, and 1 case was cultured in streptococcus vestibularis, Bacteroides uniformis and Proteus mirabilis respectively. During the follow-up, 1 patient died of cardiovascular disease 3 years after discharge, and the remaining 10 patients survived. There was no recurrence of intracranial and middle ear lesions. Sigmoid sinus and transverse sinus thrombosis were significantly improved.Conclusion Brain abscess, intracranial infection and thrombophlebitis are the most common otogenic intracranial complications, and cholesteatoma of middle ear is the most common primary disease. Timely diagnosis, multidisciplinary collaboration, accurate grasp of the timing in the treatment of primary focal and complications have improved the cure rate of the disease.
-

-
[1] 杨华, 陈晓巍, 高志强, 等. 耳源性颅内并发症临床特点分析[J]. 中华耳鼻咽喉头颈外科杂志, 2008, 43(11): 801-805. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHER202003017.htm
[2] 王晓茜, 吴佩娜, 黄宏明, 等. 发生颅外并发症的鼓膜完整的中耳病变分析[J]. 中华耳鼻咽喉头颈外科杂志, 2016, 51(5): 343-347.
[3] Duarte MJ, Kozin ED, Barshak MB, et al. Otogenic brain abscesses: A systematic review[J]. Laryngoscope Investig Otolaryngol, 2018, 3(3): 198-208. doi: 10.1002/lio2.150
[4] 杨东辉, 梁敏志, 陈声伟. 耳源性颅内并发症的临床分析[J]. 中国眼耳鼻喉科杂志, 2012, 4(12): 212-215. https://www.cnki.com.cn/Article/CJFDTOTAL-YRBH201204004.htm
[5] 单廷, 陈义钢, 洪波, 等. W-3鱼油脂肪乳在胃癌根治术后肠外营养支持治疗中的应用价值[J]. 中华消化外科杂志, 2019, 18(10): 960-965. doi: 10.3760/cma.j.issn.1673-9752.2019.10.012
[6] Saat R, Laulajainen-Hongisto AH, Mahmood G, et al. MR imaging features of acute mastoiditis and their clinical relevance[J]. AJNR Am J Neuroradiol, 2015, 36(2): 361-367. doi: 10.3174/ajnr.A4120
[7] 陈树斌, 杨本涛, 于子龙, 等. 耳源性乙状窦血栓性静脉炎CT及MRI表现[J]. 中国耳鼻咽喉头颈外科, 2018, 2(25): 79-82. https://www.cnki.com.cn/Article/CJFDTOTAL-EBYT201802007.htm
[8] 刘群, 刘衡, 朱克文, 等. MRI及磁共振静脉血管成像诊断脑静脉窦血栓形成[J]. 中国医学影像技术, 2011, 27(6): 1121-1124. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYXX201106010.htm
[9] 黎金葵, 雷军强, 杨品, 等. 磁共振静脉成像对脑静脉窦血栓诊断价值的Meta分析[J]. 中国医学影像学杂志, 2015, 23(11): 876-880. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYYZ201511025.htm
[10] 金贤德. 探讨关于脑静脉窦血栓的核磁诊断价值[J]. 齐齐哈尔医学院学报, 2015, 36(18): 2701-2702. https://www.cnki.com.cn/Article/CJFDTOTAL-QQHB201609025.htm
[11] 陆金山, 艾合买提江·艾力江, 艾帕都拉·艾斯拉, 等. 耳源性乙状窦血栓性静脉炎的诊治分析[J]. 临床耳鼻咽喉头颈外科杂志, 2023, 37(2): 116-121. doi: 10.13201/j.issn.2096-7993.2023.02.008
[12] 马修尧, 刘彬, 任超, 等. 脑动脉瘤术后腰大池置管引流患者颅内感染及影响因素[J]. 中国感染及控制杂志, 2019, 18(7): 660-664. https://www.cnki.com.cn/Article/CJFDTOTAL-GRKZ201907010.htm
[13] 张金蓉, 魏章英, 崔吉宏. 重型颅脑损伤并发颅内感染患者肺部感染的影响因素及病原学特点[J]. 中华医院感染学杂志, 2019, 29(9): 1363-1366. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHYY201909019.htm
[14] Lee MR, Pawlowski KS, Luong A, et al. Biofilm presence in humans with chronic suppurative otitis media[J]. Otolaryngol Head Neck Surg, 2009, 141(5): 567-571.
[15] Ropposch T, Nemetz U, Braun EM, et al. Management of otogenic sigmoid sinus thrombosis[J]. Otol Neurotol, 2011, 32(7): 1120-1123.
[16] 张敏, 颜旭东, 纪彩丽, 等. 耳源性颅内并发症20例临床诊疗分析[J]. 中华耳科学杂志, 2020, 18(3): 513-516. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHER202003017.htm
[17] 温鑫, 宋英鸾, 权珊, 等. 儿童中耳胆脂瘤合并颅内外并发症1例[J]. 临床耳鼻咽喉头颈外科杂志, 2022, 36(2): 139-141. doi: 10.13201/j.issn.2096-7993.2022.02.013
[18] 邓敏锋, 柯以铨. 细菌性颅内感染实验室诊断的新进展[J]. 中华神经医学杂志, 2013, 12(4): 430-432.
[19] Orji FT, Ukaegbe O, Alex-Okoro J, et al. The changing epidemiological and complications profile of chronic suppurative otitis media in a developing country after two decades[J]. Eur Arch Otorhinolaryngol, 2016, 273(9): 2461-2466.
[20] Tandon S, Beasley N, Swift AC. Changing trends in intracranial abscesses secondary to ear and sinus disease[J]. J Laryngol Otol, 2009, 123(3): 283-288.
[21] Brouwer MC, Tunkel AR, McKhann GM 2nd, et al. Brain abscess[J]. N Engl J Med, 2014, 371(5): 447-456.
[22] 柴亮, 胡静, 毛永军, 等. 耳源性颅内感染临床分析[J]. 中华耳鼻咽喉头颈外科杂志, 2018, 10(53): 770-775. https://www.cnki.com.cn/Article/CJFDTOTAL-SXYY200306031.htm
[23] Wanna GB, Dharamsi LM, Moss JR, et al. Contemporary management of intracranial complications of otitis media[J]. Otol Neurotol, 2010, 31(1): 111-117.
[24] 中华医学会神经病学分会, 中华医学会神经病学分会脑血管病学组. 中国颅内静脉系统血栓形成诊断和治疗指南2015[J]. 中华神经科杂志, 2015, 48(10): 819-829. https://www.cnki.com.cn/Article/CJFDTOTAL-XDJB201611006.htm
-




 下载:
下载: