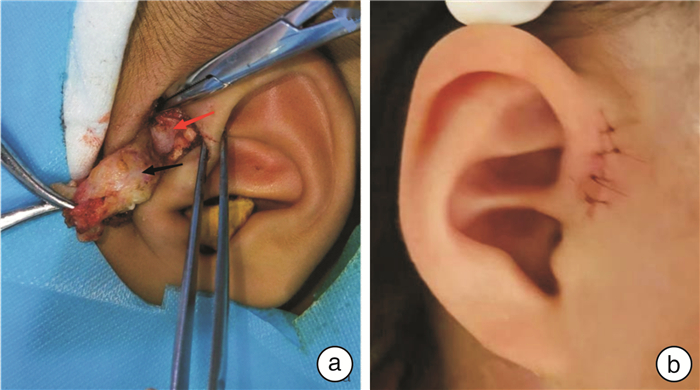
One-stage operation surgical efficacy observation of congenital preauricular fistula infection and static period of inflammation in children
-
摘要: 目的 比较感染局限期与炎症静止期小儿先天性耳前瘘管行手术治疗的临床效果。方法 选取2020年1月—2022年12月我院收治的40例先天性耳前瘘管感染局限期患儿为实验组,另选取同期收治的39例先天性耳前瘘管炎症静止期患儿作为对照组。年龄1~14岁,2组患儿瘘口均位于耳轮脚前或耳轮脚,且均为单侧瘘管,根据其瘘口及感染灶情况设计合适的切口及切除方式。术后随访6个月~2年,比较2组的疗效。结果 2组手术治疗的Ⅰ期愈合率、Ⅱ期愈合率比较差异无统计学意义(P>0.05)。2组治疗术后瘘管复发率及对耳前瘢痕满意情况,差异无统计学意义(P>0.05)。2组术后住院时间比较差异无统计学意义(P>0.05)。结论 小儿先天性耳前瘘管在感染局限期行手术治疗,与在炎症静止期施以手术治疗的效果相似,且可以减轻患儿局部麻醉换药痛苦,避免二次手术,同时降低经济成本,该治疗方法值得临床推广。Abstract: Objective To compare the clinical effect of surgical treatment of congenital preauricular fistulas in children during the local infection period and static inflammatory period.Methods Forty children with congenital preauricular fistula infection treated in our hospital from January 2020 to December 2022 were selected as the experimental group, and 39 children with congenital preauricular fistula inflammation at static period were selected as the control group. The fistula of the two groups of children aged between 1-14 years old was located in front of the foot of the ear wheel or the foot of the ear wheel, and all were unilateral fistulas. The postoperative follow-up was 6 months to 2 years, and the efficacy of the two groups was compared.Results There was no significant difference in the healing rate of stage Ⅰ and stage Ⅱ between the two groups(P>0.05). There was no significant difference in fistula recurrence rate and satisfaction with the preauricular scar between the two groups after treatment(P>0.05). There was no significant difference in postoperative hospital stay between the experimental group and the control group(P>0.05).Conclusion The effect of surgical treatment of congenital preauricular fistula in the infected period is similar to that of surgical treatment in the static period of inflammation, and it can reduce the pain of dressing change under local anesthesia in children, avoid the second operation in children, and reduce the economic cost. This treatment method is worthy of clinical promotion. Appropriate incision and resection method were designed according to the fistula and infection sites.
-

-
[1] Kim MS, Choi SW, Lee SH, et al. Surgical treatment of preauricular sinus in children: Temporalis muscle fascia anchoring suture[J]. Int J Pediatr Otorhinolaryngol, 2020, 138: 110340. doi: 10.1016/j.ijporl.2020.110340
[2] 朱雅颖, 李辰龙, 施宇轩, 等. 先天性耳前瘘管的诊治进展[J]. 中国眼耳鼻喉科杂志, 2019, 19(1): 11-15. https://www.cnki.com.cn/Article/CJFDTOTAL-YRBH201901008.htm
[3] 华娜, 卫来, 姜涛, 等. 感染性先天性耳前瘘管病理组织学观察[J]. 临床耳鼻咽喉头颈外科杂志, 2014, 28(16): 1229-1232. doi: 10.13201/j.issn.1001-1781.2014.16.013
[4] 陈布衣, 金涛, 汪超, 等. 耳前瘘管合并感染脓肿期手术切除的疗效观察[J]. 中国耳鼻咽喉颅底外科杂志, 2019, 25(3): 297-299. https://www.cnki.com.cn/Article/CJFDTOTAL-ZEBY201903017.htm
[5] 王晓锋, 李嘉, 张志雄, 等. 感染期和非感染期先天性耳前瘘管患者行手术治疗的临床效果比较[J]. 中国当代医药, 2020, 27(9): 98-100. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGUD202009029.htm
[6] 郑宽祎, 李志峰, 秦甫, 等. 先天性耳前瘘管手术时机的选择和手术方法的应用经验[J]. 临床耳鼻咽喉头颈外科杂志, 2011, 25(16): 755-756. doi: 10.3969/j.issn.1001-1781.2011.16.011
[7] 邓海燕, 高兴强, 郭宇峰. 双梭形切口手术治疗儿童感染期先天性耳前瘘管[J]. 中国耳鼻咽喉颅底外科杂志, 2021, 27(5): 582-584. https://www.cnki.com.cn/Article/CJFDTOTAL-ZEBY202105019.htm
[8] 娄丽娜. 显微外科技术在先天性耳前瘘管治疗中的应用探讨[J]. 中国医疗器械信息, 2019, 25(19): 122-123. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGQX201919055.htm
[9] 张迪, 覃纲, 赵冲, 等. 耳前组织整块切除术治疗难治性耳前瘘管[J]. 中华耳科学杂志, 2014, 12(2): 304-306. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHER201402033.htm
[10] Prasad S, Grundfast K, Milmoe G. Management of congenital preauricular pit and sinus tract in children[J]. Laryngoscope, 1990, 100(3): 320-321.
[11] 谭新华, 倪鑫, 孙浩, 等. 感染破溃型耳前瘘管单切口逆行手术切除[J]. 临床耳鼻咽喉头颈外科杂志, 2023, 37(2): 103-106. doi: 10.13201/j.issn.2096-7993.2023.02.005
-




 下载:
下载: