Clinical characteristics and efficacy of oropharyngeal carcinoma with secondary primary tumor
-
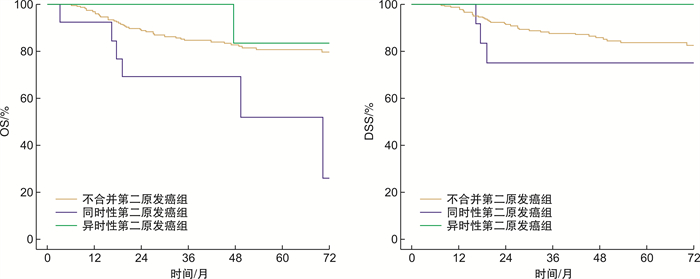
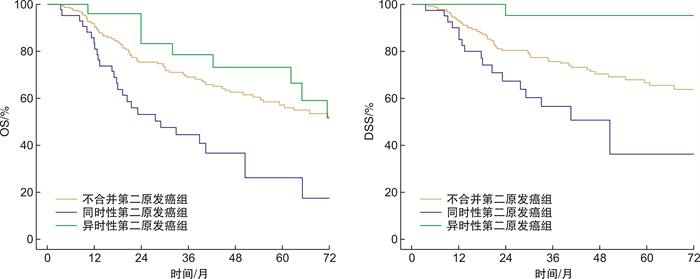
摘要: 目的 在真实世界中分析口咽癌合并第二原发肿瘤的临床特征及预后。方法 回顾性分析2010年1月至2020年12月中国医学科学院肿瘤医院收治的468例经病理证实,排除远转移,明确p16状态的以口咽为首发肿瘤的患者,分析合并第二原发肿瘤的临床特征及预后。结果 468例初治口咽癌患者,其中p16阴性222例,中位随访时间64.3个月,66例(29.3%)发生第二原发癌,其中42例(63.6%)为同时性,24例(36.4%)为异时性,食管为最常见累及部位,p16阴性口咽癌合并同时性第二原发癌、异时性第二原发癌组和无第二原发癌3组的5年生存率(overall survival OS)分别为26.3%,57.3%和73.2%(P=0.001);第二原发癌占全组死因的11.2%(12/107),其中异时性第二原发占75.0%(9/12)。p16阳性246例,中位随访时间52.4个月,20例(8.1%)发生了第二原发癌,其中13例(65.0%)为同时性,7例(35.0%)为异时性,食管为最常见累及部位,p16阳性同时性第二原发癌组和不合并第二原发癌组4年OS分别为51.9% vs 80.7%(P=0.006);p16阳性同时性第二原发癌组和合并异时性第二原发癌组4年OS分别51.9% vs 83.3%(P=0.068)。第二原发癌占全组死因的3.8%(2/52)。结论 p16阴性口咽癌发生第二原发癌概率高于p16阳性患者。无论p16状态,合并同时性第二原发癌的生存差于不合并第二原发癌组;食管均为最常见累及部位;p16阴性口咽癌,合并异时性第二原发癌预后较好,第二原发癌是其主要死因之一。Abstract: Objective To analysis the clinical features and prognosis in oropharyngeal carcinoma with secondary primary tumor.Methods A retrospective analysis was performed on 468 pathologically confirmed oropharyngeal cancer as the primary tumor patients with p16 status, excluded distant metastasis, and admitted to the Chinese Academy of Medical Sciences from January 2010 to December 2020. The clinical features and prognosis of the secondary primary tumor were analyzed.Results Among 468 patients with oropharyngeal cancer treated at initial diagnosed, 222 cases were P16-negative. With a median follow-up time of 64.3 months, 66 cases developed second primary cancer, with an incidence of 29.3%, among which 63.6%(42/66) were synchronous and 36.4%(24/66) were heterochronous, esophagus was the most commonly involved site. The 5-year OS of p16-negative oropharyngeal carcinoma with synchronous second primary cancer, without second primary cancer and with heterogeneous second primary cancer were 26.3% and 57.3% and 73.2%(P=0.001); The second primary cancer accounted for 11.2%(12/107) of the deaths in the whole group, among them, the heterochronous second primary accounted for 75.0%(9/12). There were 246 patients with p16 positive, with a median follow-up time of 52.4 months, 20 patients developed second primary cancer(8.1%). Among them, 65.0%(13/20) were synchronous and 35.0%(7/20) were heterochronous. Esophagus was the most commonly involved site. The 4-year OS of p16-positive with synchronous, heterochronous and non-second primary cancer group were 51.9%, 80.7% and 83.3%. Secondary primary cancer accounted for 3.8%(2/52) of all deaths in p16 positvie group.Conclusion The incidence of second primary cancer of p16 positive and negative oropharyngeal carcinoma were different. The esophagus was the most commonly involved site regardless of p16 status. Regardless of p16 status, the survival of patients with synchronous second primary cancer was worse than those without second primary cancer. For p16-negative oropharyngeal carcinoma, the prognosis was better in patients with heterogeneous second primary cancer, the second primary cancer is one of the main causes of death.
-

-
表 1 222例p16阴性口咽癌患者一般临床资料
例(%) 项目 全组
(222例)不合并第二原发癌
(156例)合并第二原发癌(66例) P 同时性原位癌(17例) 同时性浸润癌(25例) 异时性原位癌(7例) 异时性浸润癌(17例) 年龄/岁 56.1
(24.0~85.0)58.4
(36.0~84.0)59.9
(43.0~78.0)56.6
(45.0~69.0)51.1
(44.0~62.0)55.9
(49.0~65.0)0.118 性别 0.252 男 210(94.6) 144(92.3) 17(100.0) 25(100.0) 7(100.0) 17(100.0) 女 12(5.4) 12(7.7) 0(0) 0(0) 0(0) 0(0) ECOG 0.366 0 71(32.0) 51(32.7) 3(4.2) 7(28.0) 5(71.4) 5(29.4) 1 127(57.2) 86(55.1) 13(10.2) 16(64.0) 2(28.6) 10(58.8) ≥2 24(10.8) 19(12.2) 1(5.9) 2(8.0) 0(0) 2(11.8) 临床分期 0.462 Ⅰ~Ⅲ 38(17.1) 25(16.0) 2(11.8) 4(16.0) 3(42.9) 4(23.5) ⅣA 127(57.2) 88(56.4) 11(64.7) 13(52.0) 4(57.1) 11(64.7) ⅣB 57(25.7) 43(27.6) 4(23.5) 8(32.0) 0(0) 2(11.8) 治疗策略 0.554 手术为主 38(17.1) 28(17.9) 2(11.8) 2(8.0) 2(28.6) 4(23.5) 放疗为主 184(82.9) 128(82.1) 15(88.2) 23(92.0) 5(71.4) 13(76.5) 体重指数 0.361 < 18.5 kg/m2 13(5.9) 10(6.4) 0(0) 3(12.0) 0(0) 0(0) ≥18.5 kg/m2 209(94.1) 146(93.6) 17(100.0) 22(88.0) 7(100.0) 17(100.0) 吸烟状态 0.042 PY≤20 75(33.8) 60(38.5) 4(23.5) 9(36.0) 0(0) 2(11.8) PY>20 147(66.2) 96(61.5) 13(76.5) 16(64.0) 7(100.0) 15(88.2) 饮酒 0.004 否 227(42.0) 210(47.9) 1(5.9) 1(4.0) 0(0) 4(23.5) 是 314(58.0) 228(52.1) 16(94.1) 24(96.0) 7(100.0) 13(76.5) 表 2 246例p16阳性口咽癌患者一般临床资料
例(%) 项目 全组
(246例)不合并第二原发癌
(226例)合并第二原发癌(20例) P 同时性第二原发癌
(13例)异时性第二原发癌
(7例)年龄/岁 55.60(24.00~85.00) 56.13(24.00~85.00) 57.10(30.00~78.00) 56.50(44.00~71.00) 0.901 性别 0.194 男 187(76.0) 171(75.7) 12(92.3) 4(57.1) 女 59(24.0) 55(24.3) 1(7.7) 3(69.5) ECOG 0.021 0 101(41.1) 96(42.5) 2(15.4) 3(42.9) 1 131(53.3) 120(53.1) 8(61.5) 3(42.9) ≥2 14(5.7) 10(4.4) 3(23.1) 1(14.3) 临床分期 0.580 Ⅰ~Ⅱ 147(59.8) 137(60.6) 6(46.2) 4(57.1) Ⅲ 99(40.2) 89(39.4) 7(53.8) 3(42.9) 治疗策略 0.960 手术为主 21(13.0) 29(12.8) 2(15.4) 1(14.3) 放疗为主 214(87.0) 197(87.2) 11(84.6) 6(85.7) 体重指数 0.512 < 18.5 kg/m2 7(2.8) 6(2.7) 1(7.7) 0(0) ≥18.5 kg/m2 239(97.2) 220(97.3) 12(92.3) 7(100.0) 吸烟状态 0.026 PY≤15 160(65.3) 151(67.1) 4(30.8) 5(71.4) PY>15 85(34.7) 74(32.9) 9(69.2) 2(28.6) 饮酒 0.002 否 144(58.8) 139(61.8) 1(7.7) 4(57.1) 是 101(41.2) 86(38.2) 12(92.3) 3(42.9) 表 3 222例p16阴性口咽癌患者第二原发癌累及部位
个(%) 部位 总体
(66例)原位(同时+异时性)
(24例)浸润癌(42例) 同时性
(25例)异时性
(17例)食管 37(52.9) 13(48.2) 18(69.3) 6(35.3) 头颈部 24(34.3) 12(44.4) 6(23.1) 6(35.3) 肺 5(7.1) 0(0) 1(3.8) 4(23.5) 胃 1(1.4) 1(3.7) 0(0) 0(0) 甲状腺 1(1.4) 0(0) 1(3.8) 0(0) 结直肠 1(1.4) 1(3.7) 0(0) 0(0) 脑部 1(1.4) 0(0) 0(0) 1(5.9) 表 4 246例p16阳性口咽癌患者第二原发癌累及部位
个(%) 部位 总体
(20例)原位(同时+异时性)
(2例)浸润癌(18例) 同时性
(12例)异时性
(6例)食管 6(28.5) 1(50.0) 5(38.4) 0(0) 头颈部 4(19.0) 1(50.0) 2(15.4) 1(16.7) 肺 4(19.0) 0(0) 1(7.7) 3(49.9) 胃 1(4.8) 0(0) 1(7.7) 0(0) 甲状腺 3(14.3) 0(0) 2(15.4) 1(16.7) 前列腺癌 1(4.8) 0(0) 1(7.7) 0(0) 肝癌 1(4.8) 0(0) 1(7.7) 0(0) 十二指肠 1(4.8) 0(0) 0(0) 1(16.7) 表 5 222例p16阴性口咽癌患者中死亡患者死因分布
例(%) 项目 全组 不合并第二原发组 合并第二原发组 同时性原位癌 同时性浸润癌 异时性原位癌 异时性浸润癌 口咽癌 68(66.7) 47(69.1) 8(66.7) 11(73.3) 1(50.0) 1(10.0) 第二原发癌 12(11.2) 0(0) 0(0) 3(20.0) 1(50.0) 8(80.0) 其他 27(25.2) 21(30.9) 4(33.3) 1(6.7) 0(0) 1(10.0) 表 6 246例p16阳性口咽癌患者中死亡患者死因分布
例(%) 项目 全组 不合并第二原发组 合并第二原发组 同时性第二原发 异时性第二原发 口咽癌 35(67.3) 32(71.1) 3(50.0) 0(0) 第二原发癌 2(3.8) 1(2.2) 0(0) 1(100.0) 其他 15(28.9) 12(26.7) 3(50.0) 0(0) -
[1] Liu J, Yang XL, Zhang SW, et al. Correction to: Incidence, mortality, and temporal patterns of oropharyngeal cancer in China: a population-based study[J]. Cancer Commun(Lond), 2019, 39(1): 6.
[2] Machiels JP, René Leemans C, Golusinski W, et al. Squamous cell carcinoma of the oral cavity, larynx, oropharynx and hypopharynx: EHNS-ESMO-ESTRO Clinical Practice Guidelines for diagnosis, treatment and follow-up[J]. Ann Oncol, 2020, 31(11): 1462-1475. doi: 10.1016/j.annonc.2020.07.011
[3] Marur S, D'Souza G, Westra WH, et al. HPV-associated head and neck cancer: a virus-related cancer epidemic[J]. Lancet Oncol, 2010, 11(8): 781-789. doi: 10.1016/S1470-2045(10)70017-6
[4] Liu J, Yang XL, Zhang SW, et al. Correction to: Incidence, mortality, and temporal patterns of oropharyngeal cancer in China: a population-based study[J]. Cancer Commun(Lond), 2019, 39(1): 6.
[5] Xu T, Shen C, Wei Y, et al. Human papillomavirus(HPV)in Chinese oropharyngeal squamous cell carcinoma(OPSCC): A strong predilection for the tonsil[J]. Cancer Med, 2020, 9(18): 6556-6564. doi: 10.1002/cam4.3339
[6] Wiest T, Schwarz E, Enders C, et al. Involvement of intact HPV16 E6/E7 gene expression in head and neck cancers with unaltered p53 status and perturbed pRb cell cycle control[J]. Oncogene, 2002, 21(10): 1510-1517. doi: 10.1038/sj.onc.1205214
[7] Shi W, Kato H, Perez-Ordonez B, et al. Comparative prognostic value of HPV16 E6 mRNA compared with in situ hybridization for human oropharyngeal squamous carcinoma[J]. J Clin Oncol, 2009, 27(36): 6213-6221. doi: 10.1200/JCO.2009.23.1670
[8] Fakhry C, Lacchetti C, Rooper LM, et al. Human Papillomavirus Testing in Head and Neck Carcinomas: ASCO Clinical Practice Guideline Endorsement of the College of American Pathologists Guideline[J]. J Clin Oncol, 2018, 36(31): 3152-3161. doi: 10.1200/JCO.18.00684
[9] Moertel CG. Multiple primary malignant neoplasms: historical perspectives[J]. Cancer, 1977, 40(4 Suppl): 1786-1792.
[10] Chen MC, Chen PT, Chan CH, et al. Second primary esophageal or lung cancer in patients with head and neck carcinoma in Taiwan: incidence and risk in relation to primary index tumor site[J]. J Cancer Res Clin Oncol, 2011, 137(1): 115-123. doi: 10.1007/s00432-010-0865-0
[11] Muto M, Hironaka S, Nakane M, et al. Association of multiple Lugol-voiding lesions with synchronous and metachronous esophageal squamous cell carcinoma in patients with head and neck cancer[J]. Gastrointest Endosc, 2002, 56(4): 517-521. doi: 10.1016/S0016-5107(02)70436-7
[12] Milliet F, Bozec A, Schiappa R, et al. Synchronous primary neoplasia in patients with oropharyngeal cancer: Impact of tumor HPV status. A GETTEC multicentric study[J]. Oral Oncol, 2021, 112: 105041. doi: 10.1016/j.oraloncology.2020.105041
[13] Saito Y, Ebihara Y, Ushiku T, et al. Negative human papillomavirus status and excessive alcohol consumption are significant risk factors for second primary malignancies in Japanese patients with oropharyngeal carcinoma[J]. Jpn J Clin Oncol, 2014, 44(6): 564-569. doi: 10.1093/jjco/hyu042
[14] Jain KS, Sikora AG, Baxi SS, et al. Synchronous cancers in patients with head and neck cancer: risks in the era of human papillomavirus-associated oropharyngeal cancer[J]. Cancer, 2013, 119(10): 1832-1837. doi: 10.1002/cncr.27988
-




 下载:
下载: