Correlation between video head impulse test parameters and DHI score in patients with vestibular neuritis
-
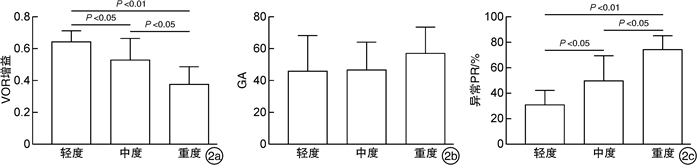
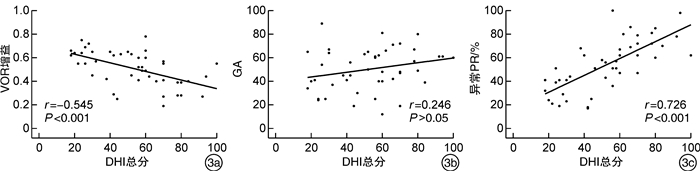
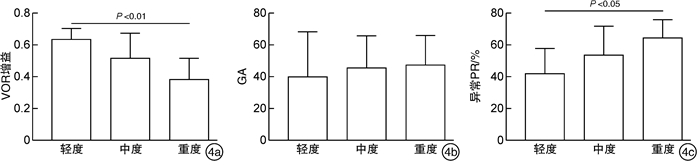
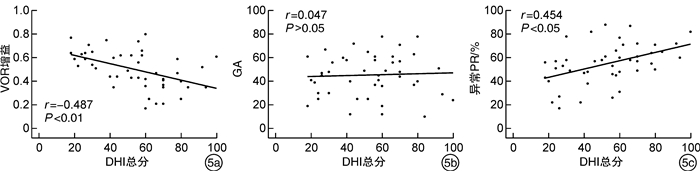
摘要: 目的探讨前庭神经炎患者视频头脉冲试验(vHIT)各参数与眩晕障碍量表(DHI)评分的相关性。方法选取前庭神经炎患者46例,询问病史,进行耳镜及听力学检查后,再行DHI量表评估和vHIT检查。按DHI得分将所有患者分为轻度眩晕组、中度眩晕组和重度眩晕组,比较三组患者的vHIT各项参数如前庭眼反射增益、增益相对不对称比(GA)、异常扫视波离散度(PR%)之间的差异。结果46例患者中,轻度眩晕组10例,中度眩晕组21例,重度眩晕组15例。①在水平管VOR增益均值对比中,轻度、中度和重度眩晕组患者vHIT增益分别为0.64±0.06、0.53±0.11、0.37±0.10,三组间VOR增益均值与DHI评分呈负相关(r=-0.545,P < 0.001),三组间两两对比均差异有统计学意义(P < 0.05)。在水平管GA均值对比中,轻度、中度和重度眩晕组患者GA分别为46.40±21.81、47.59±15.17、56.57±17.39,三组间GA均值与DHI评分无明显线性相关(r=0.246,P>0.05),三组间两两对比均差异无统计学意义(P>0.05)。在水平管PR%均值对比中,轻度、中度和重度眩晕组患者PR%均值分别为32.00±10.62、53.82±17.09、76.00±10.01,PR%与DHI评分呈明显正相关(r=0.726,P < 0.001),三组间对比均差异有统计学意义(P < 0.05)。②在垂直管VOR增益均值对比中,轻度、中度和重度眩晕组患者vHIT增益分别为0.63±0.66、0.52±0.15、0.38±0.16,三组间VOR增益均值与DHI评分呈负相关(r=-0.487,P < 0.01),轻度与重度、中度与重度眩晕组比较差异有统计学意义(P < 0.05),轻度与中度眩晕组比较差异无统计学意义(P>0.05)。在垂直管GA均值对比中,轻度、中度、重度眩晕组患者GA均值分别为40.40±15.31、46.10±19.59、47.87±18.05,三组间GA均值与DHI评分无明显线性相关(r=0.047,P>0.05),三组间GA均值对比均差异无统计学意义(P>0.05)。在垂直管PR%均值对比中,轻度、中度和重度眩晕组患者PR%均值分别为42.40±15.39、54.14±17.60、64.93±10.95,PR%与DHI评分呈明显正相关(r=0.454,P < 0.05),轻度与重度眩晕组比较差异有统计学意义(P < 0.05),其余组间比较差异无统计学意义(P>0.05)。结论前庭神经炎患者vHIT的VOR增益、PR%与DHI量表评分密切相关,可评估患者前庭功能和眩晕程度。Abstract: ObjectiveTo explore the correlation between the parameters of video head impulse test (vHIT)and dizziness handicap inventory (DHI) score in patients with vestibular neuritis.MethodsClinical data of 46 patients with vestibular neuritis were retrospectively analyzed. All the patients underwent DHI evaluation and vHIT examination. They were divided into mild handicap group, moderate handicap group and severe handicap group according to DHI score. The correlations between the parameters of vHIT and DHI score were compared among the three groups. The important parameters of vHIT were compared including vestibulo-ocular reflex (VOR) gain, gain asymmetry ratio (GA), abnormal saccade dispersion (PR%).ResultsOf the 46 patients, 10 were in the mild handicap group, 21 in the moderate handicap group, and 15 in the severe handicap group. ①In the comparison of the mean value of lateral semicircular canal VOR gain, the vHIT gain of patients with mild, moderate and severe handicap were 0.64±0.06, 0.53±0.11 and 0.37±0.10, respectively, the mean value of VOR gain was negatively correlated with DHI score among the three groups(r=-0.545, P < 0.001), and the pairwise comparisons among the three groups was statistically significant(P < 0.05). In comparison of the mean values of lateral semicircular canal GA, the GA values of mild, moderate and severe handicap groups were 46.40±21.81, 47.59±15.17 and 56.57±17.39, respectively, there was no significant linear correlation between GA values and DHI scores among the three groups(r=0.246, P>0.05), there was no significant difference between the three groups(P>0.05). In comparison of the mean PR% of the lateral semicircular canal, the mean PR% of patients with mild, moderate and severe handicap group were 32.00±10.62, 53.82±17.09 and 76.00±10.01, respectively, PR% was positively correlated with DHI score(r=0.726, P < 0.001), and the comparison among the three groups was statistically significant(P < 0.05). ②The vertical semicircular canal vHIT gain of patients with mild, moderate and severe handicap was 0.63±0.06, 0.52±0.15 and 0.38±0.16, respectively, the mean of VOR gain was negatively correlated with DHI score among the three groups(r=-0.487, P < 0.01), the comparison of mild-severe and moderate-severe group was statistically significant(P < 0.05), while there was no significant difference between the mild and moderate group(P>0.05). In the comparison of the mean values of vertical semicircular canal GA, the GA values of mild, moderate and severe handicap groups were 40.40±15.31, 46.10±19.59 and 47.87±18.05, respectively, there was no significant linear correlation between GA values and DHI scores among the three groups(r=0.047, P>0.05), there was no significant difference in GA among the three groups(P>0.05). The PR% of patients with mild, moderate and severe handicap were 42.40±15.39, 54.14±17.60 and 64.93±10.95, respectively, there was a positive significant correlation between PR% and DHI score(r=0.454, P < 0.05), there was statistically significant in the comparison of mild-severe group(P < 0.05), while there was no statistical significance between the other groups(P>0.05).ConclusionThe VOR gain and PR% value of vHIT in patients with vestibular neuritis are closely related to the DHI score, which can evaluate the vestibular function and the degree of vertigo.
-

-
[1] Tokle G, Mørkved S, Bråthen G, et al. Efficacy of Vestibular Rehabilitation Following Acute Vestibular Neuritis: A Randomized Controlled Trial[J]. Otol Neurotol, 2020, 41(1): 78-85. doi: 10.1097/MAO.0000000000002443
[2] Strupp M, Mandalà M, López-Escámez JA. Peripheral vestibular disorders: an update[J]. Curr Opin Neurol, 2019, 32(1): 165-173. doi: 10.1097/WCO.0000000000000649
[3] Welgampola MS, Taylor RL, Halmagyi GM. Video Head Impulse Testing[J]. Adv Otorhinolaryngol, 2019, 82: 56-66.
[4] Weber KP, Aw ST, Todd MJ, et al. Horizontal head impulse test detects gentamicin vestibulotoxicity[J]. Neurology, 2009, 72(16): 1417-1424. doi: 10.1212/WNL.0b013e3181a18652
[5] 丁雷, 刘畅, 王嘉玺, 等. 眩晕残障程度评定量表(中文版)的评价[J]. 中华耳科学杂志, 2013, 11(2): 228-230. doi: 10.3969/j.issn.1672-2922.2013.02.014
[6] 中国医师协会神经内科分会眩晕专业委员会, 中国卒中学会卒中与眩晕分会, 李斐, 等. 前庭神经炎诊治多学科专家共识[J]. 中华老年医学杂志, 2020, 39(9): 985-994. doi: 10.3760/cma.j.issn.0254-9026.2020.09.001
[7] 李姗姗, 韩曦, 王巍, 等. 前庭神经炎患者半规管损伤频率特征分析[J]. 临床耳鼻咽喉头颈外科杂志, 2019, 33(3): 216-219. https://www.cnki.com.cn/Article/CJFDTOTAL-LCEH201903008.htm
[8] Weber KP, Rosengren SM. Clinical utility of ocular vestibular-evoked myogenic potentials(oVEMPs)[J]. Curr Neurol Neurosci Rep, 2015, 15(5): 22. doi: 10.1007/s11910-015-0548-y
[9] Blödow A, Pannasch S, Walther LE. Detection of isolated covert saccades with the video head impulse test in peripheral vestibular disorders[J]. Auris Nasus Larynx, 2013, 40(4): 348-351. doi: 10.1016/j.anl.2012.11.002
[10] Anson ER, Bigelow RT, Carey JP, et al. VOR Gain Is Related to Compensatory Saccades in Healthy Older Adults[J]. Front Aging Neurosci, 2016, 8: 150.
[11] Whitney SL, Wrisley DM, Brown KE, et al. Is perception of handicap related to functional performance in persons with vestibular dysfunction?[J]. Otol Neurotol, 2004, 25(2): 139-143. doi: 10.1097/00129492-200403000-00010
[12] Bisdorff AR, Staab JP, Newman-Toker DE. Overview of the International Classification of Vestibular Disorders[J]. Neurol Clin, 2015, 33(3): 541-550. doi: 10.1016/j.ncl.2015.04.010
[13] 袁庆, 李昕英, 张悦, 等. 前庭神经炎视频头脉冲测试结果的动态变化[J]. 临床耳鼻咽喉头颈外科杂志, 2020, 34(11): 990-992, 998. https://www.cnki.com.cn/Article/CJFDTOTAL-LCEH202011007.htm
[14] Korsager L, Schmidt JH, Faber C, et al. Reliability and comparison of gain values with occurrence of saccades in the EyeSeeCam video head impulse test(vHIT)[J]. Eur Arch Otorhinolaryngol, 2016, 273(12): 4273-4279. doi: 10.1007/s00405-016-4183-2
[15] Du Y, Ren L, Liu X, et al. The characteristics of vHIT gain and PR score in peripheral vestibular disorders[J]. Acta Otolaryngol, 2021, 141(1): 43-49. doi: 10.1080/00016489.2020.1812715
[16] 崔庆佳, 王蕊, 闫瑾, 等. 前庭外周性眩晕患者前庭康复短期疗效及其影响因素[J]. 临床耳鼻咽喉头颈外科杂志, 2022, 36(3): 217-221. https://www.cnki.com.cn/Article/CJFDTOTAL-LCEH202203013.htm
-




 下载:
下载: