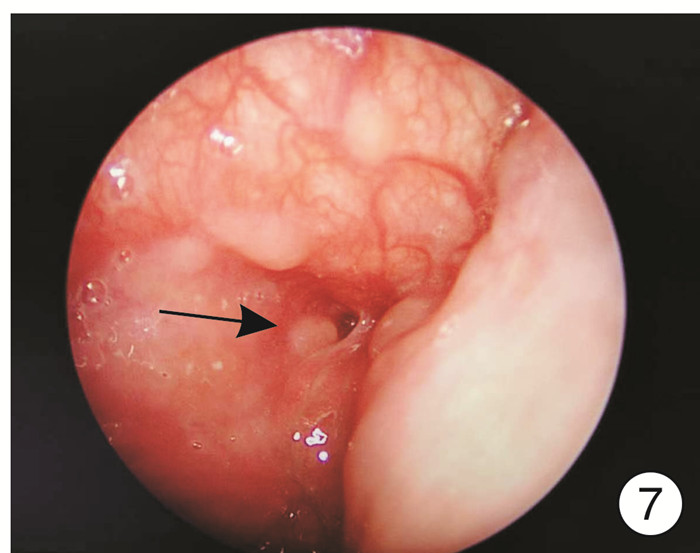
A preliminary study on low temperature plasma obliteration for pyriform sinus fistula by visual laryngoscope
-
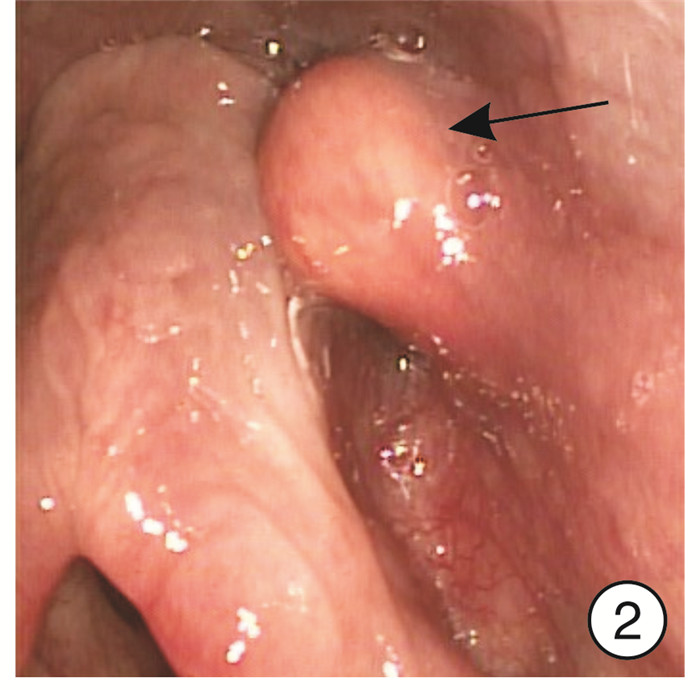
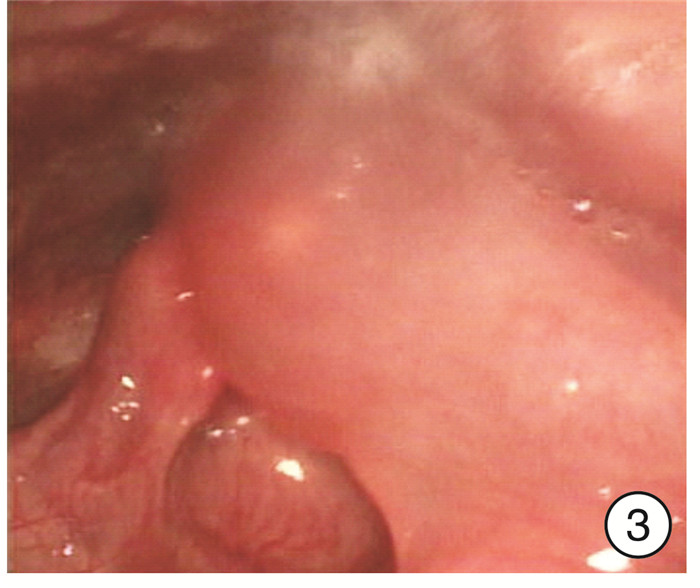
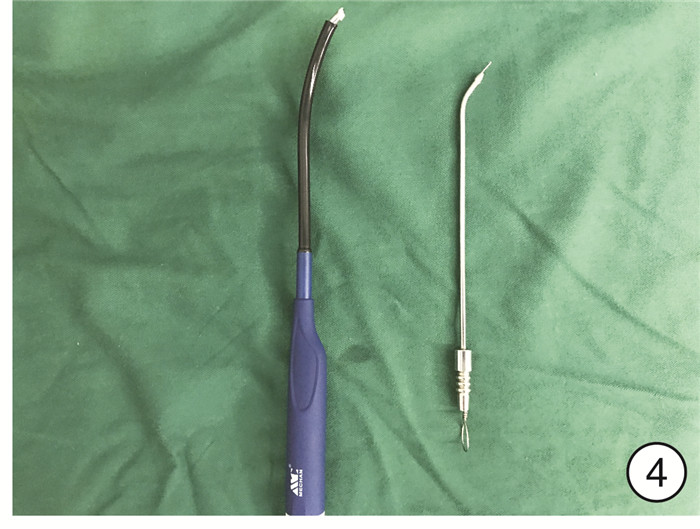
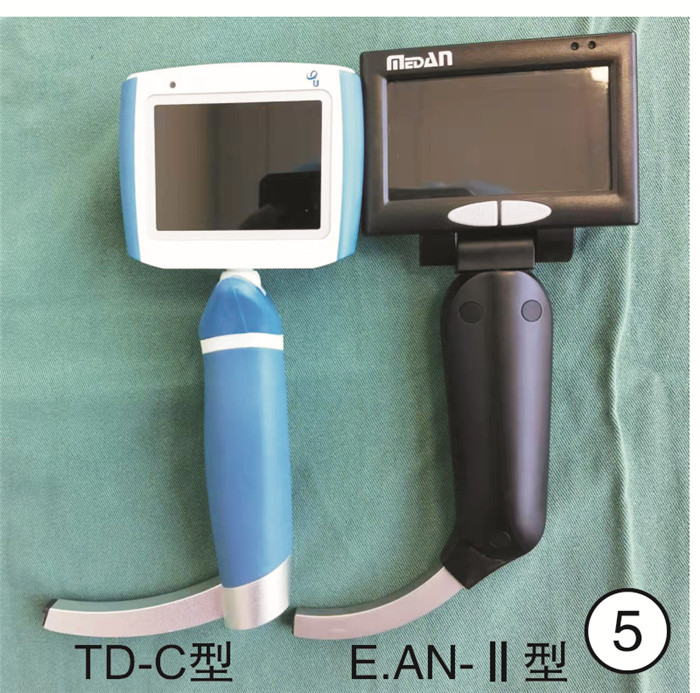
摘要: 目的 探讨可视喉镜下梨状窝瘘内口低温等离子封闭术的手术效果。方法 回顾性分析2019年3月—2021年8月在南京医科大学附属儿童医院耳鼻咽喉头颈外科行可视喉镜下梨状窝瘘内口低温等离子封闭术的29例先天性梨状窝瘘患儿的临床资料。19例行梨状窝瘘探查+瘘口封闭术,6例行梨状窝瘘探查+瘘口封闭术+颈部脓肿切开引流,4例颈部质硬包块者行梨状窝瘘探查+瘘口封闭术。术后均留置胃管。结果 所有患儿术后无严重并发症,2例出现术后声嘶,1个月后自行恢复。随访2~30个月,平均16个月,均无复发。结论 可视喉镜下梨状窝瘘内口低温等离子封闭术是一种安全有效的手术方式,创伤小,住院时间短,可作为治疗梨状窝瘘的首选术式,颈部脓肿切开引流和内口封闭可同时进行。Abstract: Objective To investigate the effect of low-temperature plasma obliteration for pyriform sinus fistula by visual laryngoscope.Methods The clinical data of 29 cases with congenital pyriform sinus fistula receiving low temperature plasma obliteration by visual laryngoscope during March 2019 to August 2021 was retrospectively analyzed in department of Otolaryngology Head and Neck Surgery of Children's Hospital of Nanjing Medical University. Nineteen cases accepted the pyriform sinus fistula probing + fistula obliteration, 6 cases accepted the pyriform sinus fistula probing + fistula obliteration + neck abscess incision and drainage, and 4 cases with cervical abscess accepted the pyriform sinus fistula probing + fistula obliteration.Results All cases had no obvious complications. Two cases had vocal cord impairment after operations and recovered after one month. There was no recurrence in 2 to 30 months follow up, with mean 16 months follow up.Conclusion Low-temperature plasma obliteration of pyriform sinus fistula by visual laryngoscope is a safe and effective surgical method with little trauma and short hospital stay. It could be the first choice for the treatment of pyriform sinus fistula. Incision and drainage of neck abscess and pyriform sinus fistula obliteration could be performed concurrently.
-
Key words:
- congenital pyriform sinus fistula /
- low temperature plasma /
- laryngoscope
-

-
表 1 29例CPSF患儿的基本资料
例序 性别 年龄 症状 起病时间/月 既往颈部脓肿切开引流次数/次 本次住院感染控制情况 手术方式 随访时间/月 1 男 4岁10个月 颈部脓肿 0.7 1 已控制 A 30 2 女 3岁 反复颈部脓肿 12.0 2 脓肿 B 21 3 女 12岁4个月 反复颈部脓肿 4.0 2 已控制 A 28 4 男 2岁8个月 颈部脓肿 1.0 1 已控制 A 25 5 男 3岁10个月 颈部脓肿 1.0 0 脓肿 B 25 6 男 4岁11个月 颈部脓肿 2.0 1 已控制 A 23 7 女 4岁5个月 颈部脓肿 1.0 1 已控制 A 23 8 男 2岁6个月 颈部脓肿 1.0 1 左颈部仍有质硬包块 A 27 9 男 9岁2个月 反复颈部红肿 4.0 0 已控制 A 23 10 女 9岁5个月 颈部无痛性包块 1.0 1 已控制a) A 18 11 男 8岁2个月 颈部红肿 1.0 0 已控制 A 18 12 男 5岁8个月 反复颈部脓肿 24.0 3 已控制 A 19 13 男 3岁10个月 颈部脓肿 0.3 0 脓肿 B 19 14 男 4岁7个月 颈部脓肿 1.0 1 已控制 A 16 15 女 7岁8个月 反复颈部脓肿 60.0 2 左颈部仍有质硬包块 A 16 16 男 6岁 颈部脓肿 0.5 1 脓肿 B 15 17 男 8岁4个月 颈部脓肿 0.5 1 已控制 A 15 18 男 5岁4个月 颈部红肿 0.5 0 左颈部仍有质硬包块 A 15 19 女 12岁11个月 反复颈部脓肿 84.0 4 已控制 A 13 20 男 3岁2个月 反复颈部脓肿 3.0 1 脓肿 B 10 21 女 8岁2个月 颈部红肿 1.0 0 已控制 A 10 22 女 2岁7个月 颈部脓肿 1.0 1 已控制 A 11 23 男 3岁3个月 颈部红肿 1.0 0 左颈部仍有质硬包块 A 10 24 女 4岁5个月 颈部红肿 0.7 0 已控制 A 6 25 女 11岁4个月 反复颈部脓肿 60.0 3 已控制 A 8 26 女 1岁7个月 颈部红肿 0.7 0 已控制 A 6 27 女 9岁6个月 颈部无痛性包块 15.0 1 已控制b) A 7 28 女 7岁4个月 颈部红肿 6.0 0 已控制 A 3 29 女 2岁11个月 颈部脓肿 1.0 0 脓肿 B 2 注:a)外院误诊为甲状舌管囊肿,切开引流后炎症控制;b)外院误诊为甲状腺结节,术中发现脓液,切开引流后炎症控制。A:梨状窝瘘探查+瘘口封闭;B:脓肿切开引流+梨状窝瘘探查+瘘口封闭。 -
[1] 刘涛, 温哲, 梁奇峰, 等. 儿童梨状窝瘘的诊断和治疗[J]. 中华医学杂志, 2016, 96(39): 3156-3159. doi: 10.3760/cma.j.issn.0376-2491.2016.39.009
[2] Lachance S, Chadha NK. Systematic Review of Endoscopic Obliteration Techniques for Managing Congenital Piriform Fossa Sinus Tracts in Children[J]. Otolaryngol Head Neck Surg, 2016, 154(2): 241-246. doi: 10.1177/0194599815613286
[3] Nicoucar K, Giger R, Pope HG Jr, et al. Management of congenital fourth branchial arch anomalies: a review and analysis of published cases[J]. J Pediatr Surg, 2009, 44(7): 1432-1439. doi: 10.1016/j.jpedsurg.2008.12.001
[4] Nicoucar K, Giger R, Jaecklin T, et al. Management of congenital third branchial arch anomalies: a systematic review[J]. Otolaryngol Head Neck Surg, 2010, 142(1): 21-28. e2. doi: 10.1016/j.otohns.2009.09.001
[5] Derks LS, Veenstra HJ, Oomen KP, et al. Surgery versus endoscopic cauterization in patients with third or fourth branchial pouch sinuses: A systematic review[J]. Laryngoscope, 2016, 126(1): 212-217. doi: 10.1002/lary.25321
[6] Cha W, Cho SW, Hah JH, et al. Chemocauterization of the internal opening with trichloroacetic acid as first-line treatment for pyriform sinus fistula[J]. Head Neck, 2013, 35(3): 431-435. doi: 10.1002/hed.22998
[7] Wong PY, Moore A, Daya H. Management of third branchial pouch anomalies-an evolution of a minimally invasive technique[J]. Int J Pediatr Otorhinolaryngol, 2014, 78(3): 493-498. doi: 10.1016/j.ijporl.2013.12.027
[8] Wang L, Sang J, Zhang Y, et al. Evaluation of endoscopic coblation treatment for obliteration of congenital pyriform sinus fistula[J]. Acta Otolaryngol, 2018, 138(6): 574-578. doi: 10.1080/00016489.2017.1420916
[9] Chen W, Chen J, Chen F, et al. Endoscopic coblation treatment for congenital pyriform sinus fistula in children[J]. Medicine(Baltimore), 2021, 100(19): e25942. https://pubmed.ncbi.nlm.nih.gov/34106664/
[10] 中国妇幼保健学会微创分会儿童耳鼻咽喉学组. 儿童先天性梨状窝瘘诊断与治疗临床实践指南[J]. 临床耳鼻咽喉头颈外科杂志, 2020, 34(12): 1060-1064. https://www.cnki.com.cn/Article/CJFDTOTAL-LCEH202012002.htm
[11] 马静, 明澄, 娄凡, 等. 儿童先天性梨状窝瘘的误诊原因分析及治疗方法探讨[J]. 中华耳鼻咽喉头颈外科杂志, 2018, 53(5): 381-384. doi: 10.3760/cma.j.issn.1673-0860.2018.05.010
[12] Miyauchi A, Matsuzuka F, Kuma K, et al. Piriform sinus fistula: an underlying abnormality common in patients with acute suppurative thyroiditis[J]. World J Surg, 1990, 14(3): 400-405. doi: 10.1007/BF01658538
[13] Hao Z, Hou Y, Li X, et al. Misdiagnosis of asymptomatic intrathyroidal pyriform sinus fistula: a case report[J]. J Int Med Res, 2021, 49(7): 3000605211031430. https://pubmed.ncbi.nlm.nih.gov/34282642/
-




 下载:
下载: