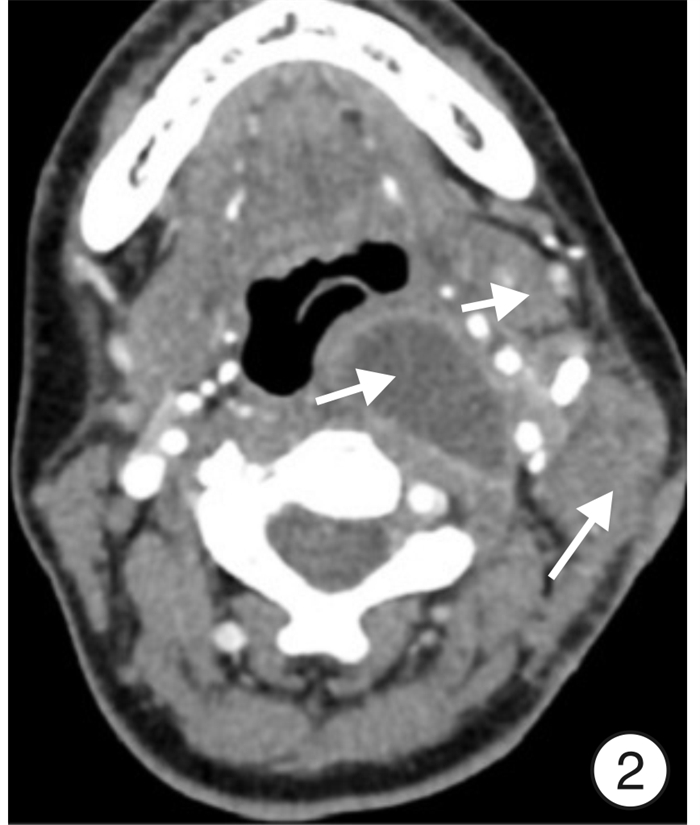
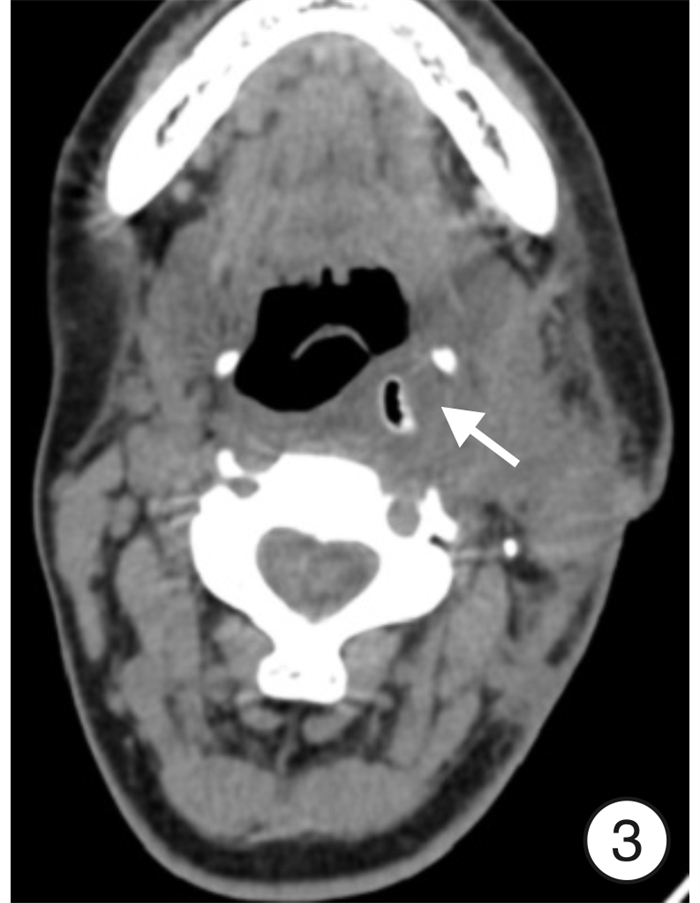
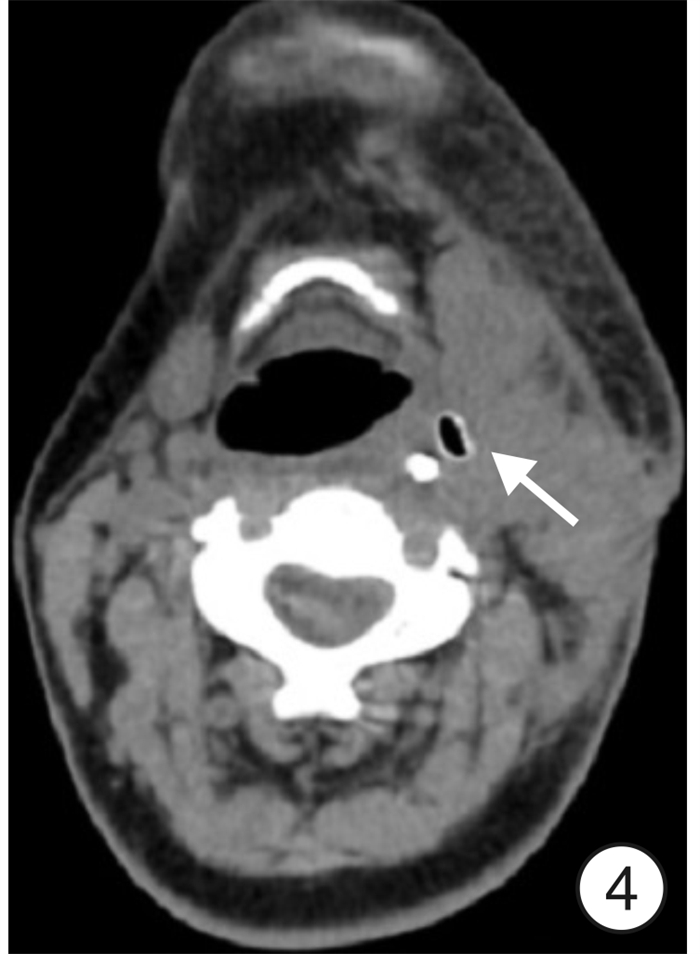
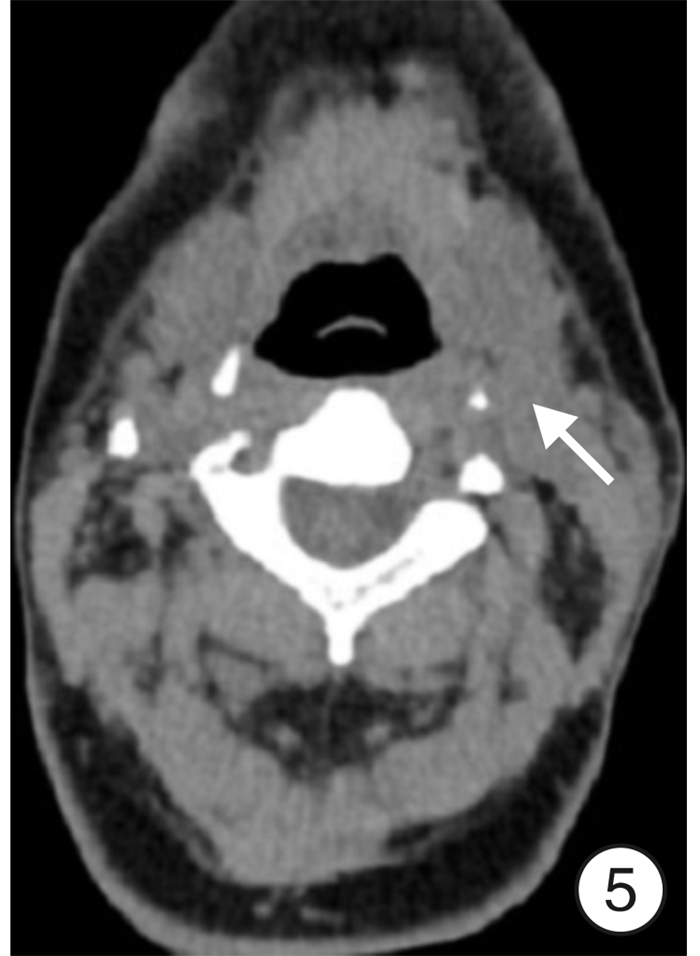
Clinical analysis of lateral cervical approach in the treatment of cervical lymphatic tuberculosis complicated with parapharyngeal space abscess
-
摘要: 目的 探讨颈侧径路治疗颈部淋巴结核合并咽旁间隙脓肿的临床疗效。 方法 对10例明确诊断为颈部淋巴结核合并咽旁间隙脓肿患者采取颈侧径路手术治疗, 记录患者手术时间和出血量, 对比术前与术后2周血沉、C反应蛋白(CRP)、VAS评分、洼田饮水试验评级, 比较术前、术后2周和末次随访时的切口愈合情况, 结核中毒症状的变化, 颈部CT术区部位变化等情况。 结果 10例患者手术时间65 ~130 min, 平均(99.00 ± 21.45) min; 术中出血量100~250 mL, 平均(155.00±43.78) mL。入院时血沉为(67.60± 21.94) mm/1h, 术后2周为(30.30±13.76) mm/1h, 差异有统计学意义(U=5.500, P<0.01); 入院时CRP为(69.70 ±31.13) mg/ L, 术后2周为(42.40±19.70) mg/L(U=22.500, P<0.05); 术前VAS评分为(5.60 ± 1.26) 分, 术后2周为(2.50±1.27) 分(U=4.500, P<0.01)。洼田饮水试验术后2周评级均在1 ~2级之间, 解除压迫后, 饮水均无明显呛咳, 并在2次以内咽下。10例患者随访6~24个月, 随访期间手术伤口愈合良好, 全身结核中毒症状消失, 复查颈部CT咽旁间隙无明显残腔及积液, 口咽部无明显向内突出组织, 术区周围软组织水肿基本消失, 肿大淋巴结较前明显缩小, 且无液化、坏死、化脓及复发迹象。 结论 颈侧径路手术治疗颈部淋巴结核合并咽旁间隙脓肿是一种良好的治疗方法。Abstract: Objective To investigate the clinical effect of lateral cervical approach in the treatment of cervical lymphatic tuberculosis complicated with parapharyngeal space abscess. Methods A total of 10 patients with cervical lymph node tuberculosis complicated with tuberculous abscess in parapharyngeal space were treated. Surgery was performed using a transcervical approach. The operation time and blood loss were recorded. The level of ESR, C-reactive protein(CRP), VAS score and the rating of Kubota drinking test before and 2 weeks after operation were compared. The incision healing, symptoms of tuberculosis poisoning, and the CT findings of the cervical lesions were compared before operation, 2 weeks after operation and at the last follow-up. Results The operation time ranged from 65 to 130 min with an average of (99.00±21.45) min. The intraoperative blood loss ranged from 100 to 250 mL with an average of (155.00±43.78) mL. The average pre-and post-operative level of ESR was (67.60±21.94) mm/1h and (30.30±13.76) mm/1h, respectively(U=5.500, P<0.01); The average pre-and post-operative level of CRP was (69.70±31.13) mg/L and (42.40±19.70) mg/L, respectively(U=22.500, P<0.05); The average pre-and post-operative VAS score was (5.60±1.26) points and (2.50±1.27) points, respectively(U=4.500, P<0.01). As for Kubota drinking test, the rating was between 1-2 two weeks postoperatively. After relieving the compression, there was no obvious choking and coughing in drinking water. During the follow-up period (range: 6-24 months), the surgical wound healed completely, and the symptoms of systemic tuberculosis poisoning disappeared. No obvious residual cavity or effusion was found in the parapharyngeal space by CT examination, nor was any protruding tissue in oropharynx. The edema of soft tissue surrounding the operational area disappeared, and the enlarged lymph nodes were significantly reduced. No sign of liquefaction, necrosis, suppuration or recurrence was observed. Conclusion Surgery using transcervical approach effective in treating cervical lymph node tuberculosis with parapharyngeal space abscess.
-

-
表 1 10例患者手术前后血沉、CRP及VAS评分对比
时间 血沉/
(mm·1h-1)CRP/
(mg·L-1)VAS评分/分 术前 67.60±21.94 69.70±31.13 5.60±1.26 术后2周 30.30±13.76 42.40±19.70 2.50±1.27 U 5.500 22.500 4.500 P 0.001 0.037 0.001 -
[1] 唐神结, 高文. 临床结核病学[M]. 北京: 人民卫生出版社, 2011 : 478-485.
[2] Kuet ML, Kasbekar AV, Masterson L, et al. Management of tumors arising from the parapharyngeal space: A systematic review of 1, 293 cases reported over 25 years[J]. Laryngoscope, 2015, 125 (6) : 1372- 1381. doi: 10.1002/lary.25077
[3] 侯佳欣, 王玲, 曾泉, 等. 咽旁间隙肿瘤影像学与治疗方式选择[J]. 临床耳鼻咽喉头颈外科杂志, 2020, 34 (10) : 937-941. https://www.cnki.com.cn/Article/CJFDTOTAL-LCEH202010018.htm
[4] Shukla RH, Nemade SV, Shinde KJ. Comparison of visual analogue scale(VAS)and the Nasal Obstruction Symptom Evaluation (NOSE)score in evaluation of post septoplasty patients[J]. World J Otorhinolaryngol Head Neck Surg, 2020, 6(1) : 53-58. doi: 10.1016/j.wjorl.2019.06.002
[5] 华荣誉, 杨方英, 梁冠冕. 洼田饮水试验筛检头颈部肿瘤患者吞咽障碍风险的meta分析[J]. 中国眼耳鼻喉科杂志, 2020, 20(1) : 36-40, 45. https://www.cnki.com.cn/Article/CJFDTOTAL-YRBH202001013.htm
[6] 张玥玥, 郑玲. 基于美国肿瘤放射治疗协会颈部淋巴结分区标准的转移性淋巴结影像分析[J]. 中国中西医结合影像学杂志, 2020, 18(4) : 365-368. https://www.cnki.com.cn/Article/CJFDTOTAL-JHYX202004013.htm
[7] 赵建东, 文艺, 纵亮, 等. 原发性咽旁间隙肿瘤治疗的回顾性分析[J]. 临床耳鼻咽喉头颈外科杂志, 2020, 34(8) : 743-747. https://www.cnki.com.cn/Article/CJFDTOTAL-LCEH202008015.htm
[8] 姚岚, 肖和平. 颈部淋巴结结核发生结核性脓肿的危险因素分析[J]. 中国防痨杂志, 2019, 41(1) : 53-56. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFLZ201901014.htm
[9] 王彦冬, 郝凯飞, 经翔, 等. 超声引导经皮颌下区穿刺置管引流在咽旁间隙脓肿治疗中的应用[J]. 中华超声影像学杂志, 2020, 29(11) : 977-981.
[10] Gopakumar KG, Mohan N, Prasanth VR, et al. Isolated parapharyngeal cold abscess in a 9-year-old boy [J]. Paediatr Int Child Health, 2019, 39(2) : 139-141.
[11] KoskoJ, CaseyJ. Retropharyngeal and parapharyngeal abscesses: Factors in medical management failure[J]. Ear Nose ThroatJ, 2017, 96(1) : E12-E15.
[12] 侯佳欣, 王玲, 胡国华. 咽旁间隙肿瘤手术径路及其应用解剖[J]. 中华解剖与临床杂志, 2020, 25(1) : 88-92.
[13] Patterson JM, McColl E, Carding PN, et al. Swallowing beyond six years post(chemo)radiotherapy for head and neckcancer; a cohort study[J]. Oral Oncol, 2018, 83: 53-58.
[14] Cordesmeyer R, Kauffmann P, Markus T, et al. Bacterial and histopathological findings in deep head and neck infections: a retrospective analysis[J]. Oral Surg Oral Med Oral Pathol Oral Radiol, 2017, 124 (1) : 11-15.
-




 下载:
下载: