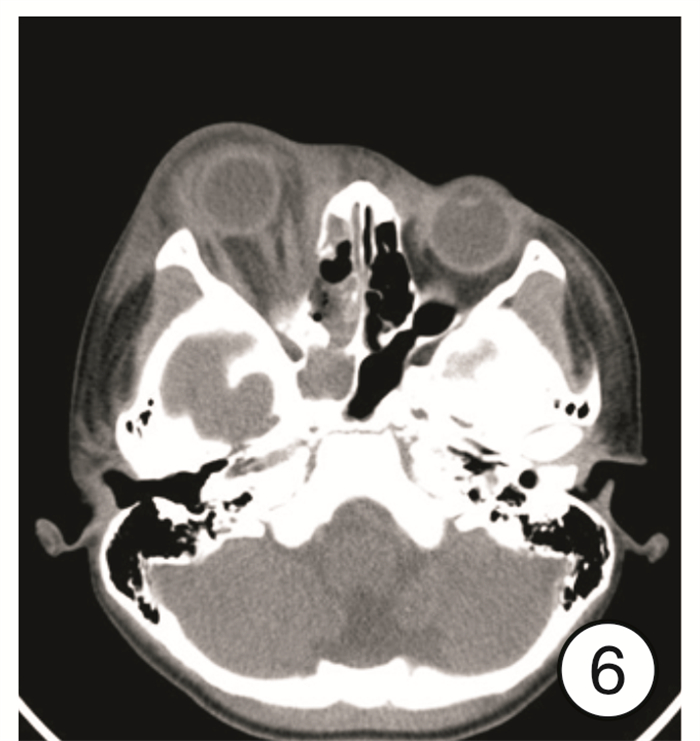
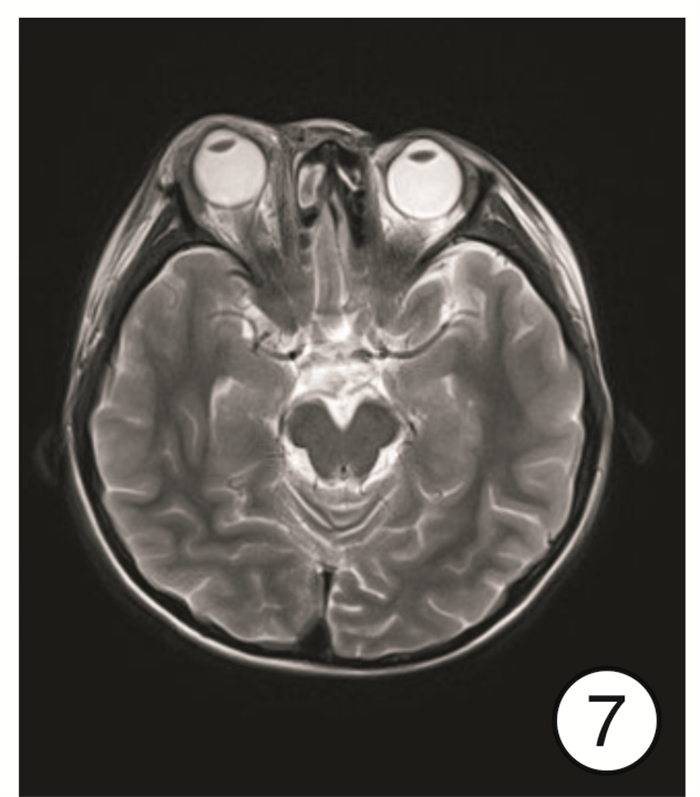
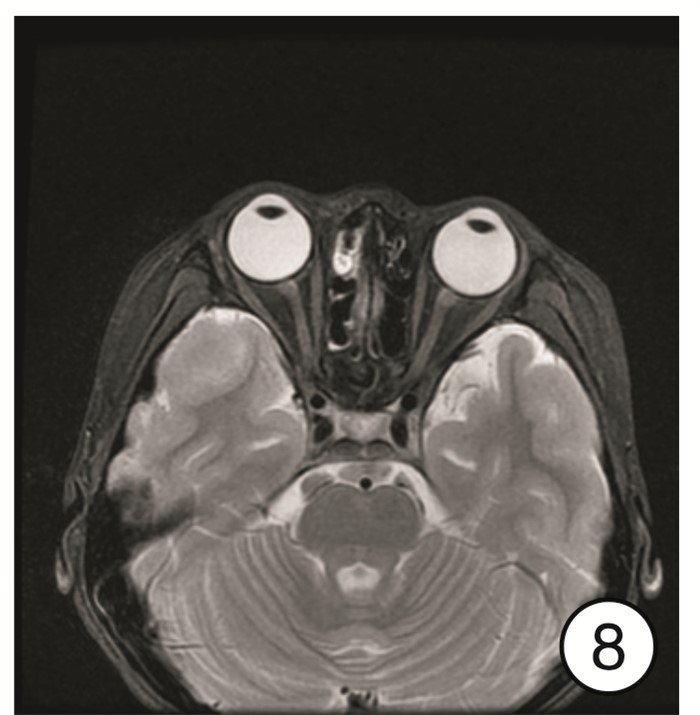
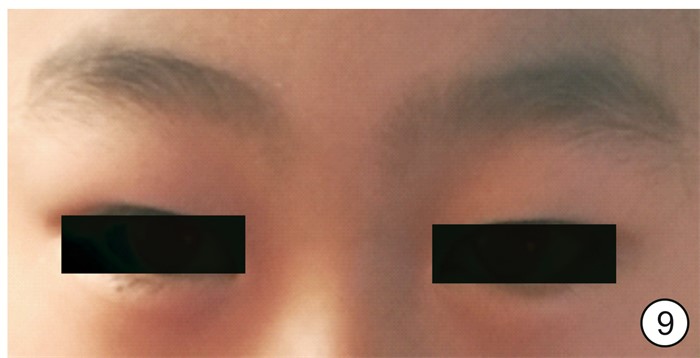
Diagnosis and treatment of 11 cases of subperiosteal orbital abscess caused by acute sinusitis
-
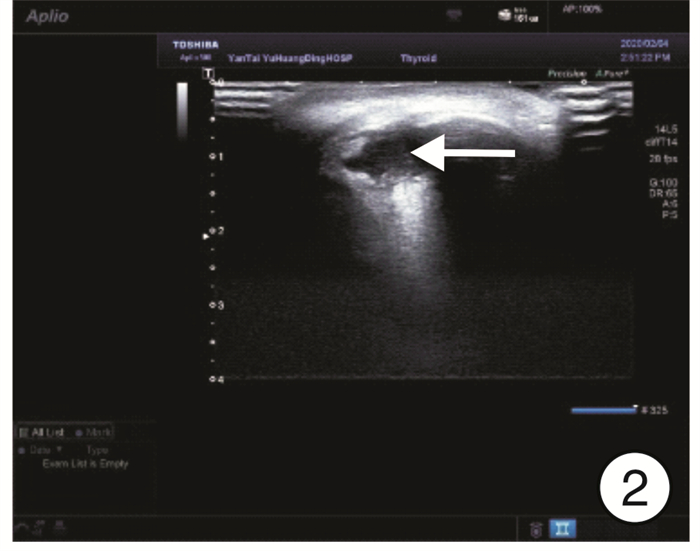
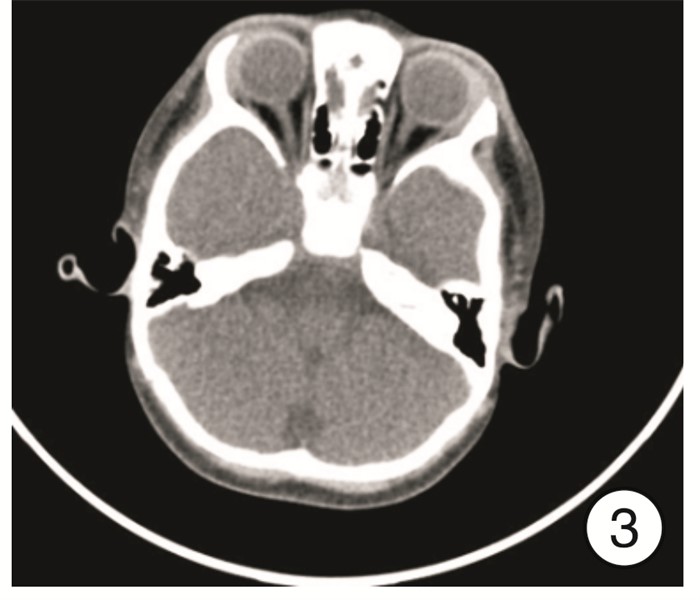
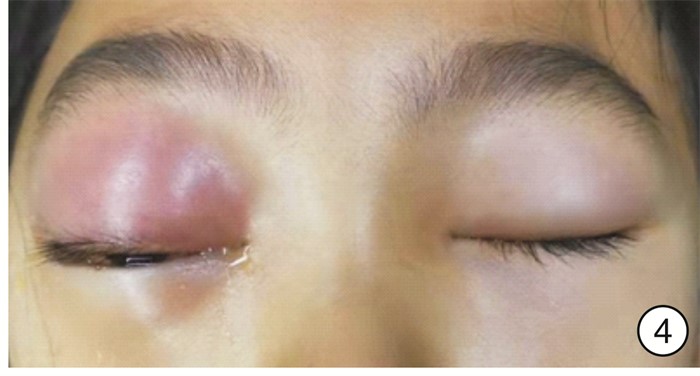
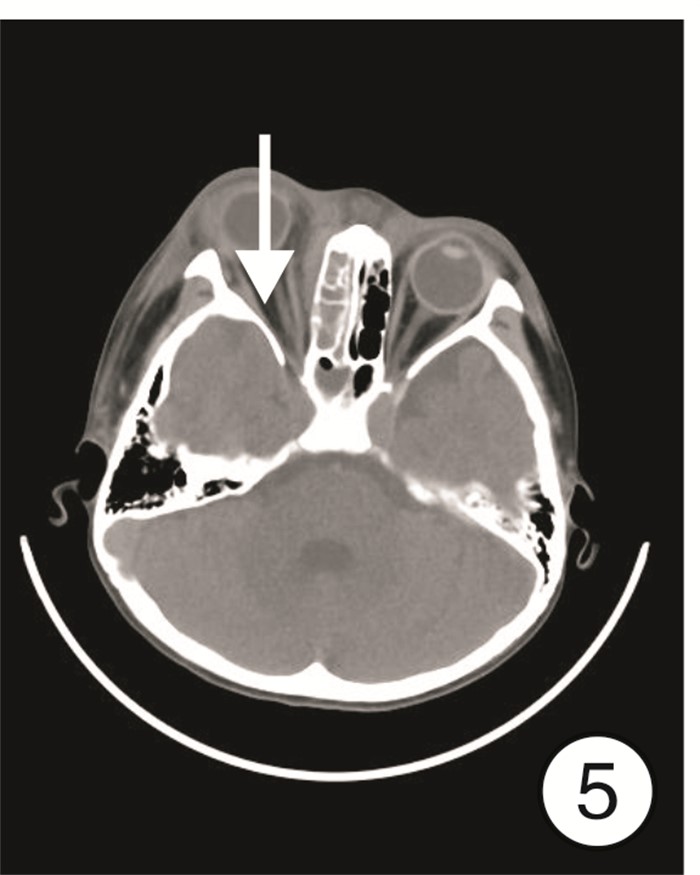
摘要: 目的 总结急性鼻窦炎并发眶骨膜下脓肿的诊断、临床表现及手术治疗经验。方法 回顾性分析11例1岁8个月~50岁急性鼻窦炎并发眶骨膜下脓肿患者的临床资料, 包括临床表现、影像学表现、细菌学检验、手术方式及治疗效果。所有患者均给予抗菌药物、糖皮质激素以及手术治疗。结果 11例患者均为单侧病变, 影像学检查均支持眶骨膜下脓肿表现, 9例患者行鼻内镜下鼻窦开放+眶骨膜下脓肿切开引流术, 2例行鼻内镜下鼻窦开放+超声引导下脓肿穿刺术。均痊愈出院, 出院时眼睑肿胀、突眼症状基本缓解, 10例患者未出现视力改变; 1例患者就诊时视力仅存光感, 出院时恢复至0.05, 随访3个月视力无变化。鼻腔分泌物或脓液细菌培养阳性者7例, 分别为金黄色葡萄球菌3例(其中1例为耐甲氧西林金黄色葡萄球菌)、咽峡炎链球菌2例、中间链球菌2例。结论 鼻源性眶骨膜下脓肿起病急, 进展快, 一旦形成脓肿, 保守治疗效果欠佳者需尽早选择手术治疗。手术方式最常见的是鼻内镜下鼻窦开放+眶骨膜下脓肿切开引流术, 若脓肿位于眼球上方或者外上方, 需结合超声引导下穿刺或切开引流。Abstract: Objective The aim of this study is to explore the diagnosis, clinical manifestations and surgical treatment experience of acute sinusitis complicated with orbital subperiosteal abscess.Methods The clinical data of 11 patients with acute sinusitis complicated by orbital subperiosteal abscess from 1 year and 8 months to 50 years were retrospectively analyzed, including clinical manifestations, imaging manifestations, bacteriological examinations, surgical methods and therapeutic effects. All patients were given antibacterial drugs, glucocorticoids, and surgery.Results All 11 patients had unilateral lesions. The imaging examinations all supported the appearance of orbital subperiosteal abscess. Nine patients underwent nasal endoscopic sinus opening+SPOA incision and drainage, 2 patients underwent nasal endoscopic sinus opening+ultrasound guided abscess puncture. Eyelid swelling and exophthalmia of all patients were alleviated when discharged. Ten of the 11 patients had no visual acuity change, and one patient had light perception only when she came to the hospital and recovered to 0.05 when discharged, there was no change in visual acuity after 3 months follow-up. The bacterial cultures of nasal secretion or pus were positive in 7 cases, the main pathogenic bacteria were Staphylococcus aureus(3 cases, includes one case of MRSA), Streptococcus anginosus(2 cases), and Streptococcus intermedius(2 cases).Conclusion Rhinogenous orbital subperiosteal abscess has a rapid onset and progresses quickly. Once an abscess is formed, patients with poor conservative treatment should choose surgical treatment as soon as possible. The most common surgical method is nasal endoscopic sinus opening+SPOA incision and drainage. If the abscess is located above or above the eyeball, puncture or incision and drainage should be combined with ultrasound guidance.
-
Key words:
- sinusitis /
- orbital abscess /
- endoscopic surgical procedures
-

-
表 1 11例患者的临床症状、体征及手术方式
例序 年龄 性别 脓肿
侧别眼球
突出眼球
活动上睑
下垂视力
下降分泌物细菌培养结果 手术方式 1 2岁2个月 男 左 无 正常 无 无 咽峡炎链球菌 第1次:鼻内镜下左侧筛窦、上颌窦开放术+超声引导下眶骨膜下脓肿穿刺术;第2次:超声引导下脓肿穿刺术 2 8岁 女 右 有 受限 有 有 金黄色葡萄球菌 鼻内镜下右侧筛窦、上颌窦、蝶窦开放+眶减压+右侧眶骨膜下脓肿切开引流术 3 3岁11个月 男 左 有 受限 有 无 金黄色葡萄球菌 鼻内镜下左侧筛窦、上颌窦开放+眶减压+左侧眶骨膜下脓肿切开引流术 4 1岁8个月 男 右 有 正常 无 无 咽峡炎链球菌 鼻内镜下右侧筛窦、上颌窦开放+眶减压+右侧眶骨膜下脓肿切开引流术 5 6岁 男 左 无 正常 无 无 金黄色葡萄球菌 鼻内镜下左侧上颌窦、筛窦、蝶窦开放+眶减压+左侧眶骨膜下脓肿切开引流术 6 15岁 男 右 有 受限 无 无 无细菌生长 鼻内镜下右侧全组鼻窦开放+眶减压+右侧眶骨膜下脓肿切开引流术 7 16岁 女 右 有 受限 有 无 中间链球菌 鼻内镜下右侧筛窦、上颌窦、额窦开放+眶减压术+超声引导下眶骨膜下脓肿穿刺置管引流术 8 25岁 男 左 有 受限 有 无 无细菌生长 鼻内镜下左侧全组鼻窦开放+眶减压+左侧眶骨膜下脓肿切开引流术 9 26岁 男 左 有 受限 无 无 无细菌生长 鼻内镜下左侧筛窦、上颌窦、蝶窦开放+眶减压+左侧眶骨膜下脓肿切开引流术 10 50岁 女 左 有 受限 无 无 无细菌生长 鼻内镜下左侧筛窦开放+眶减压+左侧眶骨膜下脓肿切开引流术 11 5岁 女 右 有 受限 无 无 中间链球菌 鼻内镜下右侧筛窦、上颌窦开放+眶减压+右侧眶骨膜下脓肿切开引流术 -
[1] Çelik M, Kaya KH, Yegin Y, et al. Anatomical Factors in Children with Orbital Complications Due to Acute Rhinosinusitis[J]. Iran J Otorhinolaryngol, 2019, 31(106): 289-295.
[2] Pradhan P, Samal DK, Preetam C, et al. Intraorbital and Intracranial Complications of Acute Rhinosinusitis: A Rare Case Report[J]. Iran J Otorhinolaryngol, 2018, 30(100): 301-304.
[3] Jabarin B, Marom T, Gavriel H, et al. Orbital complications secondary to acute rhinosinusitis in toddlers: A unique age group[J]. Int J Pediatr Otorhinolaryngol, 2019, 121: 46-49. doi: 10.1016/j.ijporl.2019.03.002
[4] Schollin Ask L, Hultman Dennison S, Stjärne P, et al. Most preschool children hospitalised for acute rhinosinusitis had orbital complications, more common in the youngest and among boys[J]. Acta Paediatr, 2017, 106(2): 268-273. doi: 10.1111/apa.13650
[5] Chandler JR, Langenbrunner DJ, Stevens ER. The pathogenesis of orbital complications in acute sinusitis[J]. Laryngoscope, 1970, 80(9): 1414-1428. doi: 10.1288/00005537-197009000-00007
[6] 王丹, 张浩, 杨素红. 儿童眼部蜂窝织炎临床分析[J]. 中国斜视与小儿眼科杂志, 2019, 27(3): 25-28. doi: 10.3969/J.ISSN.1005-328X.2019.03.008
[7] 赵亮, 唐东润, 吴桐, 等. 眼眶及眶周脓肿17例临床分析[J]. 中华眼科杂志, 2017, 53(8): 588-593. doi: 10.3760/cma.j.issn.0412-4081.2017.08.006
[8] Tsirouki T, Dastiridou AI, Ibánez Flores N, et al. Orbital cellulitis[J]. Surv Ophthalmol, 2018, 63(4): 534-553. doi: 10.1016/j.survophthal.2017.12.001
[9] Nageswaran S, Woods CR, Benjamin DK Jr, et al. Orbital cellulitis in children[J]. Pediatr Infect Dis J, 2006, 25(8): 695-699. doi: 10.1097/01.inf.0000227820.36036.f1
[10] McKinley SH, Yen MT, Miller AM, et al. Microbiology of pediatric orbital cellutitis[J]. AmJ Ophthalmol, 2007, 144(4): 497-501. doi: 10.1016/j.ajo.2007.04.049
[11] 樊云葳, 吴倩, 于刚, 等. 97例儿童眶蜂窝织炎的诊治及疗效[J]. 眼科, 2015, 24(6): 397-401. https://www.cnki.com.cn/Article/CJFDTOTAL-YAKE201506016.htm
[12] 熊娟, 陈延旭, 环梦佳, 等. 儿童眶蜂窝织炎79例诊疗分析[J]. 重庆医学, 2017, 46(20): 2831-2833. doi: 10.3969/j.issn.1671-8348.2017.20.031
[13] Pushker N, Tejwani LK, Bajaj MS, et al. Role of oral corticosteroids in orbital cellulitis[J]. Am J Ophthalmol, 2013, 156(1): 178-183. e1. doi: 10.1016/j.ajo.2013.01.031
[14] Davies BW, Smith JM, Hink EM, et al. C-Reactive Protein As a Marker for Initiating Steroid Treatment in Children With Orbital Cellulitis[J]. Ophthalmic Plast Reconstr Surg, 2015, 31(5): 364-368. doi: 10.1097/IOP.0000000000000349
[15] Chen L, Silverman N, Wu A, et al. Intravenous Steroids With Antibiotics on Admission for Children With Orbital Cellulitis[J]. Ophthalmic Plast Reconstr Surg, 2018, 34(3): 205-208. doi: 10.1097/IOP.0000000000000910
[16] Fokkens WJ, Lund VJ, Hopkins C, et al. European Position Paper on Rhinosinusitis and Nasal Polyps 2020[J]. Rhinology, 2020, 58(Suppl S29): 1-464.
[17] Tachibana T, Kariya S, Orita Y, et al. Factors that prolong the duration of recovery in acute rhinosinusitis with orbital complications[J]. Acta Otolaryngol, 2019, 139(1): 52-56. doi: 10.1080/00016489.2018.1539516
[18] Taubenslag KJ, Chelnis JG, Mawn LA. Management of frontal sinusitis-associated subperiosteal abscess in children less than 9 years of age[J]. J AAPOS, 2016, 20(6): 527-531. e1. doi: 10.1016/j.jaapos.2016.08.007
[19] Wan Y, Shi G, Wang H. Treatment of Orbital Complications Following Acute Rhinosinusitis in Children[J]. Balkan Med J, 2016, 33(4): 401-406. doi: 10.5152/balkanmedj.2016.141065
[20] Trivić A, Cevik M, Folić M, et al. Management of Orbital Complications of Acute Rhinosinusitis in Pediatric Patients: A 15-Year Single-Center Experience[J]. Pediatr Infect Dis J, 2019, 38(10): 994-998. doi: 10.1097/INF.0000000000002414
[21] Wang Y, Zhang J, Dong L, et al. Orbital abscess treated by ultrasound-guided fine needle aspiration and catheter drainage: A case report[J]. Medicine(Baltimore), 2019, 98(39): e17365.
-




 下载:
下载: