-
摘要: 目的 探讨波特氏头皮肿块(pott's puffy tumor,PPT)的临床特征及诊疗策略。方法 回顾性分析2例PPT患者的临床资料,并结合文献,着重对围手术期诊疗策略进行综合分析。2例患者均通过多学科会诊,给予及时、足量、可透过血脑屏障抗生素抗感染,及时行经鼻内镜内外联合径路PPT病变清除术。结果 2例患者经规范化围手术期处理,症状缓解,随访1年无复发。术后未出现额部疼痛及麻木感、局部凹陷、瘢痕增生等并发症。结论 PPT临床上相对罕见、病情危重,应引起重视;多学科会诊,及时、足量抗生素的使用,结合经鼻内镜内外联合径路PPT病变清除术,是规范化围手术期处理策略的关键。Abstract: Objective To explore the characteristics and therapeutic strategies of Pott's puffy tumor(PPT).Methods The clinical data of two patients with PPT were retrospectively analyzed and combined with the literature, focusing on the comprehensive analysis of perioperative diagnosis and treatment strategies. Both patients underwent muti-disciplinary treatment, including timely administration of sufficient antibiotics capable of penetrating the blood-brain barrier. Early removal of PPT lesions was performed using a combined internal and external approach under nasal endoscopic guidance.Results After standardized perioperative management, the symptoms of the two patients were completely relieved, with no recurrence after one=year follow=up. Postoperative complications such as frontal pain, numbness, local depression, or scar hyperplasiawere not present.Conclusion PPT, being relatively rare and severe, requires careful attention. Key strategies for standardized perioperative management include multi-disciplinary consultation, timely and adequate antibiotic administration, and surgical intervention using a combined intranasal and extranasal endoscopic approach for lesion removal.
-

-
[1] Yang HJ, Paik SW, Park DJ, et al. Pott Puffy Tumor Caused by Dental Infection: A Case Report and Literature Review[J]. J Craniofac Surg, 2022, 33(2): e127-e130. doi: 10.1097/SCS.0000000000008010
[2] 陈志鹏, 吴喜福, 郑博文, 等. 滑车上动脉和眶上动脉定位在内外联合径路额窦内镜手术中的应用[J]. 中华耳鼻咽喉头颈外科杂志, 2022, 57(8): 931-936.
[3] Ketenci I, Unlü Y, Tucer B, et al. The Pott's puffy tumor: a dangerous sign for intracranial complications[J]. Eur Arch Otorhinolaryngol, 2011, 268(12): 1755-1763. doi: 10.1007/s00405-011-1660-5
[4] Koltsidopoulos P, Papageorgiou E, Skoulakis C. Pott's puffy tumor in children: A review of the literature[J]. Laryngoscope, 2020, 130(1): 225-231. doi: 10.1002/lary.27757
[5] Hasan I, Smith SF, Hammond-Kenny A. Potts puffy tumour: a rare but important diagnosis[J]. J Surg Case Rep, 2019, 2019(4): rjz099.
[6] Sharma P, Sharma S, Gupta N, et al. Pott puffy tumor[J]. Proc(Bayl Univ Med Cent), 2017, 30(2): 179-181.
[7] Min HJ, Kim KS. Frontocutaneous Fistula Secondary to Pott's Puffy Tumor[J]. Ear Nose Throat J, 2020, 99(9): NP101-NP102. doi: 10.1177/0145561319856858
[8] Rohde RL, North LM, Murray M, et al. Pott's puffy tumor: A comprehensive review of the literature[J]. Am J Otolaryngol, 2022, 43(5): 103529. doi: 10.1016/j.amjoto.2022.103529
[9] Tibesar RJ, Azhdam AM, Borrelli M. Pott's Puffy Tumor[J]. Ear Nose Throat J, 2021, 100(6_suppl): 870S-872S. doi: 10.1177/01455613211039031
[10] Min HJ, Kim KS. Odontogenic Sinusitis-Associated Pott's Puffy Tumor: A Case Report and Literature Review[J]. Ear Nose Throat J, 2022, 101(4): NP186-NP188. doi: 10.1177/0145561320952203
[11] Leong SC. Minimally Invasive Surgery for Pott's Puffy Tumor: Is It Time for a Paradigm Shift in Managing a 250-Year-Old Problem?[J]. Ann Otol Rhinol Laryngol, 2017, 126(6): 433-437. doi: 10.1177/0003489417698497
[12] Pendolino AL, Koumpa FS, Zhang H, et al. Draf Ⅲ frontal sinus surgery for the treatment of Pott's puffy tumour in adults: our case series and a review of frontal sinus anatomy risk factors[J]. Eur Arch Otorhinolaryngol, 2020, 277(8): 2271-2278. doi: 10.1007/s00405-020-05980-2
-

| 引用本文: | 邓慧仪, 陈志鹏, 吴喜福, 等. 波特氏头皮肿块的临床特征及诊疗策略[J]. 临床耳鼻咽喉头颈外科杂志, 2024, 38(1): 83-85. doi: 10.13201/j.issn.2096-7993.2024.01.015 |
| Citation: | DENG Huiyi, CHEN Zhipeng, WU Xifu, et al. Characteristics and therapeutic strategies of Pott's puffy tumor[J]. J Clin Otorhinolaryngol Head Neck Surg, 2024, 38(1): 83-85. doi: 10.13201/j.issn.2096-7993.2024.01.015 |
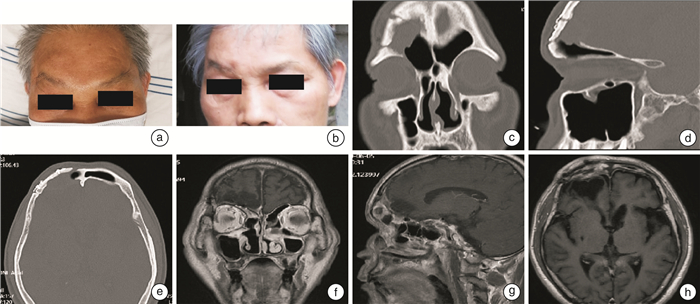
- Figure 1.
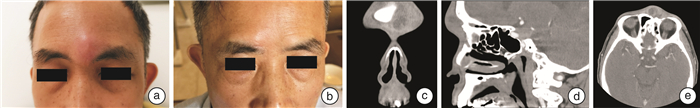
- Figure 2.



 下载:
下载: