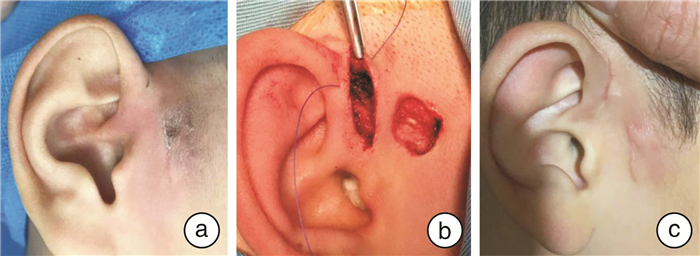
Study on the management of granulation during surgery for congenital preauricular fistula infection stage
-
摘要: 目的 探讨先天性耳前瘘管感染期术中对肉芽的处理方法及手术效果。方法 总结2018年1月至2022年9月收治的140例感染期先天性耳前瘘管患者的手术方法以及对肉芽的2种处理方法,随机分为观察组和对照组,观察组79例切除瘘管、对肉芽不予处理,对照组61例在切除瘘管的同时切除肉芽,术后随访半年,对伤口愈合、复发情况以及采用斯托尼布鲁克瘢痕评估量表评估肉芽愈合美观度。结果 140例感染期先天性耳前瘘管患者行以上2种手术方法切除,观察组与对照组的伤口愈合、复发情况比较,差异无统计学意义,观察组瘢痕更小。结论 感染期先天性耳前瘘管在手术切除瘘管的同时,无需切除肉芽,肉芽处均能良好愈合,且瘢痕反应更小。Abstract: Objective To investigate the management of granulation tissue during surgery for infected congenital preauricular fistula and to assess the surgical outcomes.Methods To summarize the surgical methods and the treatment of granulation methods in 140 cases of congenital preauricular fistula during the period of infection treated in our department from January 2018 to September 2022. The study divided patients into an observation group (79 patients) undergoing fistulectomy without granulation treatment, and a control group (61 patients) where fistulectomy and granulation resection were performed concurrently.. After six months of follow-up, the wound healing, recurrence rates, and the aesthetic assessment of granulation healing were evaluated using the Stony Brook Scar Evaluation Scale(SBSES).Results The two surgical approaches were applied to a total of 140 patients with infected congenital preauricular fistula. There was no statistical difference in wound healing and recurrence rates between the observation group and the control group. However, the observation group exhibited smaller scars.Conclusion In cases of infected congenital preauricular fistula, surgical removal without excising granulation tissue is feasible, leading to effective healing and lesser scar formation.
-
Key words:
- infection stage /
- congenital preauricular fistula /
- granulation treatment
-

-
表 1 斯托尼布鲁克瘢痕评估量表
参数内容 得分 宽度 瘢痕加宽明显,宽度>2 mm 0 瘢痕加宽不明显,宽度≤2 mm 1 厚度 瘢痕增厚明显 0 瘢痕增厚不明显 1 颜色(红色) 瘢痕红于周围皮肤 0 瘢痕色泽接近或低于周围皮肤 1 缝合痕迹 处于缝合线 0 小于缝合线 1 整体外观 差 0 好 1 表 2 观察组与对照组指标比较
组别 性别/例 侧别/例 中位年龄/岁 中位病程/d 并发症/例(%) 复发/例(%) SUSES中位评分 男 女 左 右 观察组 27 52 43 36 10(1~71) 10(3~21) 3(3.79) 1(1.26) 4(1~5) 对照组 21 40 32 29 12(2~48) 9(4~20) 4(6.55) 1(1.63) 2(0~4) P 0.975 0.969 0.685 0.809 0.846 0.855 < 0.001 -
[1] 周萍, 陈金辉, 黄婷, 等. 先天性耳前瘘管的研究进展[J]. 临床耳鼻咽喉头颈外科杂志, 2019, 33(5): 474-477. https://lceh.whuhzzs.com/article/doi/10.13201/j.issn.1001-1781.2019.05.024
[2] Pang J, Xiong H, Liao Q, et al. The diagnosis and treatment of a variant type of auricular sinus: postauricular sinus[J]. Eur Arch Otorhinolaryngol, 2019, 276(7): 1961-1967. doi: 10.1007/s00405-019-05431-7
[3] 马玉强, 刘海霞, 王勤学, 等. 童变异型耳前瘘管临床特征及手术技巧[J]. 中华耳科学杂志, 2020, 18(6): 1130-1133. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHER202006025.htm
[4] Fearmonti R, Bond J, Erdmann D, et al. A review of scar scales and scar measuring devices[J]. Eplasty, 2010, 10: e43.
[5] 高秀丽, 徐晓冰, 傅窈窈, 等. 超高频超声在先天性耳前瘘管诊断中的应用[J]. 中国眼耳鼻喉科杂志, 2021, 21(3): 185-188. https://www.cnki.com.cn/Article/CJFDTOTAL-YRBH202103010.htm
[6] 秦昊, 李嘉慧, 陈彦球, 等. 儿童变异型耳前瘘管并发耳后脓肿的手术治疗[J]. 临床耳鼻咽喉头颈外科杂志, 2022, 36(8): 621-624. https://lceh.whuhzzs.com/article/doi/10.13201/j.issn.2096-7993.2022.08.011
[7] 冀庆军, 柴伟, 冯春博, 等. 显微镜下配合消融电极手术治疗复发性先天性耳前瘘管16例[J]. 中国耳鼻咽喉头颈外科, 2022, 29(11): 736-737. https://www.cnki.com.cn/Article/CJFDTOTAL-EBYT202211012.htm
[8] 周萍, 陈金辉, 黄婷, 等. 以耳轮棘为解剖标志的精细耳前瘘管切除术疗效及复发相关因素分析[J]. 中国耳鼻咽喉头颈外科, 2019, 26(4): 194-197. https://www.cnki.com.cn/Article/CJFDTOTAL-EBYT201904007.htm
[9] 张媛霞, 宫宇. 清扫式耳前瘘管摘除术治疗耳前瘘管感染期患者的临床疗效及并发症观察[J]. 贵州医药, 2021, 45(10): 1638-1639. https://www.cnki.com.cn/Article/CJFDTOTAL-GZYI202110072.htm
[10] 王林, 胡光维. 耳前组织扩大切除术在感染期及复杂性耳前瘘管治疗中的应用[J]. 中国耳鼻咽喉头颈外科, 2021, 28(3): 182-183. https://www.cnki.com.cn/Article/CJFDTOTAL-EBYT202103015.htm
[11] 李隽, 夏忠芳, 姚薇, 等. 儿童耳前瘘管切除术不同手术方式的疗效观察[J]. 华中科技大学学报(医学版), 2021, 50(5): 626-631. https://www.cnki.com.cn/Article/CJFDTOTAL-TJYX202105015.htm
[12] 陈布衣, 金涛, 汪超, 等. 耳前瘘管合并感染脓肿期手术切除的疗效观察[J]. 中国耳鼻咽喉颅底外科杂志, 2019, 25(3): 297-299. https://www.cnki.com.cn/Article/CJFDTOTAL-ZEBY201903017.htm
[13] 汪燕, 陈玉赞. 感染期先天性耳前瘘管一期治疗与二期治疗的疗效比较[J]. 中国中西医结合耳鼻咽喉科杂志, 2020, 28, (2): 113-115. https://www.cnki.com.cn/Article/CJFDTOTAL-XYJH202002010.htm
[14] 郑立岗, 虞幼军, 陈抗松, 等. 感染期先天性耳前瘘管一期切除术[J]. 中国耳鼻咽喉颅底外科杂志, 2017, 23(6): 580-581. https://www.cnki.com.cn/Article/CJFDTOTAL-ZEBY201706023.htm
[15] 郑顺昌. 先天性耳前瘘管感染期的手术时机及技巧[J]. 临床耳鼻咽喉头颈外科杂志, 2016, 30(19): 1557-1558. https://lceh.whuhzzs.com/article/doi/10.13201/j.issn.1001-1781.2016.19.013
[16] 邓海燕, 高兴强, 郭宇峰. 双梭形切口手术治疗儿童感染期先天性耳前瘘管[J]. 中国耳鼻咽喉颅底外科杂志, 2021, 27(5): 582-584. https://www.cnki.com.cn/Article/CJFDTOTAL-ZEBY202105019.htm
[17] 张海港, 樊明月, 尹德佩, 等. "H"型切口和". "型切口在儿童感染性耳前瘘管切除术中的应用[J]. 中国耳鼻咽喉颅底外科杂志, 2021, 27(5): 585-588. https://www.cnki.com.cn/Article/CJFDTOTAL-ZEBY202105020.htm
[18] 杨素娜, 尹德佩. 应用双向推进皮瓣法进行儿童耳前瘘管切除术中皮损修复的实践[J]. 中国耳鼻咽喉头颈外科, 2023, 30(3): 157-160. https://www.cnki.com.cn/Article/CJFDTOTAL-EBYT202303005.htm
-




 下载:
下载: