Effect of maxillary expansion combined with orofacial myofunctional therapy on the position of the tongue of children with mouth breathing
-
摘要: 目的 研究骨性Ⅱ类错
-

-
表 1 口面肌功能训练方法
练习内容 练习时间及频率 具体内容 N点训练 每次10 s,5次1组,每天3组 将舌尖抵在上中切牙后5 mm或发英文字母“N”结束时舌尖的位置,维持10 s,保持小张口,唇肌放松。 唇肌训练(吹纸训练) 每次10 s,5次1组,每天3组 保持抿住双唇10 s,尽量不要露出唇红。面前放一张纸巾,用力发“泼”音,用发“泼”音的气流力量将纸吹起。 呼吸训练(左右鼻孔交替呼吸) 每次10 s,5次1组,每天3组 闭上嘴,伸出双手食指,右手食指压住右侧鼻孔,用左侧鼻孔深吸气。憋住10 s,换左手食指压住左侧鼻孔,用右侧鼻孔将气呼出,之后交换鼻孔。 弹舌训练 每组20次,每天3组 将舌吸到上腭,迅速离开上腭发出类似马蹄“哒哒”声。训练舌前部和中部肌肉,帮助舌上抬。 吞咽训练(咧嘴弹舌吞咽训练) 每组15次,每天3组 大笑状,后牙轻咬,嘴唇离开牙齿,弹舌发出响声(口底部不发声,下巴不动,牙齿保持咬合)后吞咽。 表 2 鼻呼吸组和口呼吸组舌体位置比较
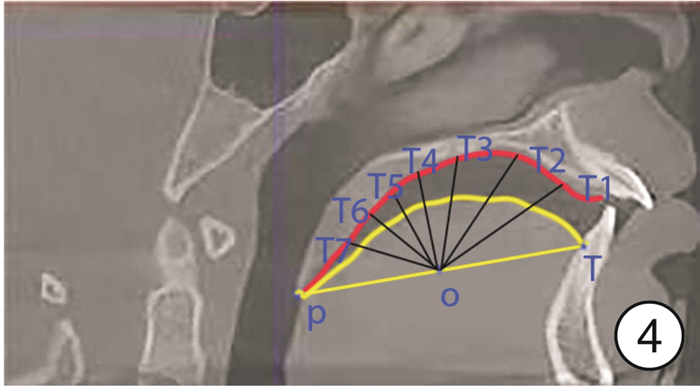
mm,X±S 测量项目 鼻呼吸组(15例) 口呼吸组(15例) P T1 0.00±0.00 5.70±3.49 0.010 T2 0.00±0.00 7.59±4.70 0.011 T3 0.00±0.00 6.59±4.30 0.013 T4 0.00±0.00 5.99±3.30 0.007 T5 0.00±0.00 4.50±3.15 0.017 T6 0.06±0.00 2.47±2.11 0.035 T7 0.04±0.00 1.51±1.24 0.031 表 3 矫治前后舌体位置比较
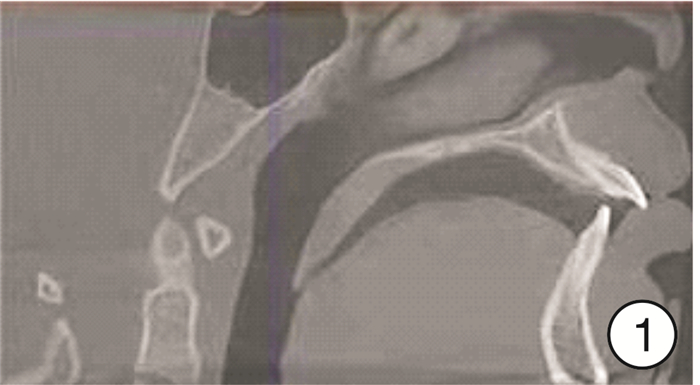
mm,X±S 测量项目 治疗前(D1) 治疗后(D2) D1-D2 P T1 5.71±3.49 0.68±1.05 5.03±3.49 0.021 T2 7.59±4.70 0.80±1.28 4.79±5.15 0.023 T3 4.59±4.30 0.83±1.30 5.74±4.51 0.024 T4 5.99±3.29 1.01±1.60 4.98±3.54 0.019 T5 4.50±3.15 1.10±1.79 3.40±3.35 0.045 T6 2.48±2.11 0.24±0.52 2.21±2.05 0.046 T7 1.50±1.23 0.00±0.00 0.00±0.00 0.031 -
[1] 严冬, 车晓霞. 口呼吸对颅面生长发育影响的研究进展[J]. 北京口腔医学, 2016, 24(2): 113-115. https://www.cnki.com.cn/Article/CJFDTOTAL-BJKX201602021.htm
[2] 贺红, 赵婷婷. 儿童错
[3] 曾祥龙, 高雪梅. 儿童口呼吸的诊断与处理[J]. 中华口腔医学杂志, 2020, 55(1): 6-6.
[4] 史真. 口面肌功能治疗临床诊疗手册[M]. 北京: 人民卫生出版社, 2016: 62-68.
[5] Kravanja SL, Hocevar-Boltezar I, Music MM, et al. Threedimensional ultrasound evaluation of tongue posture and its impact on articulation disorders in preschool children with anterior open bite[J]. Radiol Oncol, 2018, 52(3): 250-256. doi: 10.2478/raon-2018-0032
[6] Primozic J, Farcnik F, Perinetti G, et al. The association of tongue posture with the dentoalveolar maxillary and mandibular morphology in Class Ⅲ malocclusion: a controlled study[J]. Eur J Orthod, 2013, 35(3): 388-393. doi: 10.1093/ejo/cjs015
[7] Borsa L, Estève D, Charavet C, et al. Malocclusions and oral dysfunctions: A comprehensive epidemiological study on 359 schoolchildren in France[J]. Clin Exp Dent Res, 2023, 9(2): 332-340. doi: 10.1002/cre2.719
[8] 牟鸿恩, 钱玉芬. 基于锥形束CT分析骨性Ⅱ类错
[9] 臧艳姿, 娄颖, 李靖, 等. 口面肌功能训练联合肌功能矫治器在儿童OSA术后康复治疗中的应用[J]. 临床耳鼻咽喉头颈外科杂志, 2022, 36(6): 457-462. https://lceh.whuhzzs.com/article/doi/10.13201/j.issn.2096-7993.2022.06.010
[10] 卢晓峰, 朱敏. 腺样体和扁桃体肥大-张口呼吸-腺样体面容的序列治疗[J]. 临床耳鼻咽喉头颈外科杂志, 2016, 30(6): 451-454. https://www.cnki.com.cn/Article/CJFDTOTAL-LCEH201606008.htm
[11] 杨咪, 卢彩莲, 王小琴. 口呼吸青少年儿童上气道形态与舌骨位置的特征研究[J]. 中国实用口腔科杂志, 2022, 15(4): 411-415, 419. https://www.cnki.com.cn/Article/CJFDTOTAL-ZSKQ202204006.htm
[12] 郭靖晗, 於丽明, 李远远, 等. 上颌扩弓联合双
[13] de Felício CM, da Silva Dias FV, Trawitzki LVV. Obstructive sleep apnea: focus on myofunctional therapy[J]. Nat Sci Sleep, 2018, 10: 271-286.
-




 下载:
下载: