The effect of endoscopic dacryocystorhinostomy on different lacrimal duct obstruction
-
摘要: 目的 观察鼻内镜泪囊鼻腔吻合术对不同原因泪道阻塞的疗效。方法 收集80眼泪道阻塞患者,行鼻内镜泪囊鼻腔吻合术,术中同时矫正鼻腔结构异常,处理鼻腔鼻窦病变。术后随访10个月~8年。结果 一期治愈率为78.8%,有效率为17.5%,无效率为3.8%,一期成功率为96.2%。一期手术无效3眼中,2眼再次手术后治愈,总成功率为98.8%。结论 针对不同原因引起的泪道阻塞,鼻内镜泪囊鼻腔吻合术可作为常规术式,术中可同时处理鼻腔鼻窦结构异常和病变,结合术后治疗和随访,可获得长期疗效。Abstract: Objective To observe the effect of endoscopic dacryocystorhinostomy on different lacrimal duct obstruction.Methods Eighty eyes with the lacrimal passage obstruction were collected, and treated with endoscopic dacryocystorhinostomy. Meanwhile, the abnormal structures of the nasal cavity were corrected and the pathological changes of the nasal cavity and sinuses were treated. The patients were followed up and the curative effect was observed. Follow-up period ranged from 10 months to 8 years.Results The first operation cure rate was 78.8%, the effective rate was 17.5%, the ineffective rate was 3.8%, and the success rate was 96.2%. Two of the 3 eyes failed in first operation were cured by reoperation. The total success rate was 98.8%.Conclusion Endoscopic dacryocystorhinostomy can be used as a routine operation in the treatment of different lacrimal duct obstruction. The structural abnormalities and pathological changes of the nasal cavity and paranasal sinuses can be treated simultaneously. Combined with postoperative treatment and follow-up, long-term curative effect can be obtained.
-

-
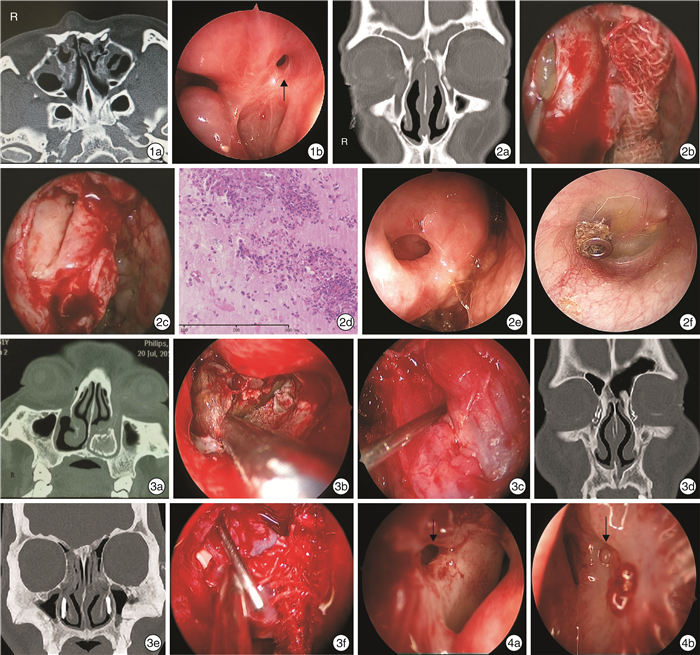
图 1 图1 双侧鼻骨及左侧上颌骨额突骨折患者术前及术后所见 1a: 水平位 CT 显示双侧鼻骨、 左侧上颌骨额突骨折, 左 侧鼻泪管阻塞;1b: 鼻内镜泪囊鼻腔吻合术后3 个月复查, 黑色箭头示吻合口; 图2 慢性鼻窦炎合并双侧泪囊炎 2a: 冠状位 CT 显示鼻窦炎合并双侧泪囊炎;2b: 切开右侧泪囊, 可见内容物为黏蛋白;2c: 清除泪囊内黏蛋白后, 可见黏 膜高度水肿;2d: 泪囊内黏蛋白病理染色可见大量嗜酸粒细胞;2e: 术后1 年半右侧泪囊鼻腔吻合口略缩窄;2f: 右侧中耳 因慢性炎症置管; 图3 泪道置管继发感染2例 3a: 病例1 冠状位 CT 显示左侧下鼻道高密度影;3b: 病例1 鼻内镜 下显示左侧下鼻道泪道置管周围被真菌团块包裹;3c: 病例1 左侧泪囊鼻腔吻合术中可见泪囊黏膜明显肿胀, 泪囊腔狭 窄, 泪道探针自泪总管开口探入泪囊;3d: 病例2 冠状位双侧泪道置管, 泪囊内置管端碎裂;3e: 病例2 双侧下鼻道可见置 管;3f: 病例2 右侧泪囊切开后可见黏膜肿胀, 探针左下方白色片状物为人工泪管残留; 图4 双侧先天性鼻泪管闭锁术后1个月 4a: 右侧吻合口(黑色箭头所示) 开放;4b: 左侧吻合口(黑色箭头所示) 闭锁。
图 5 图5 泪囊水平CT 右侧钩突附着处位于泪囊鼻腔外侧壁投影前方, 左侧位于泪囊鼻腔外侧壁投影之中; 图6 泪囊水平CT 左侧钩突气化, 位于泪囊窝鼻腔外侧壁投影之中; 图7 手术步骤 7a: 右鼻腔黏膜瓣切口位置(* 为中鼻甲, # 为鼻中隔) ;7b: 暴露右侧鼻腔外侧壁上颌骨额突鼻腔侧面, 拟行泪囊鼻腔吻合术区域;7c: 如图7a 所示区域切开并 分离右侧鼻腔外侧壁黏骨膜瓣;7d: 将黏骨膜瓣暂时翻转至嗅裂区;7e: 去除泪囊鼻腔投影区的上颌骨额突骨质和部分 泪骨;7f: 切开泪囊鼻腔侧黏膜, 将黏膜瓣与鼻腔黏膜对合;7g: 修剪置于嗅裂的黏膜瓣至合适大小, 复位覆盖于泪囊鼻腔 吻合口上方暴露的上颌骨额突骨面, 泪囊内放置膨胀海绵扩张泪囊腔;7h: 另一块膨胀海绵压迫固定黏骨膜瓣; 图8 泪道阻塞伴鼻中隔偏曲患者鼻中隔矫正术后再行鼻内镜泪囊鼻腔吻合术 8a: 冠状位 CT 示鼻中隔左偏, 左侧鼻泪管阻 塞;8b: 鼻中隔矫正术后暴露左侧泪囊, 在泪囊内侧壁上下缘各做一横切口(黑色箭头所示) ;8c: 在内侧壁中间作一纵行 切口, 形成“工”形切口;8d: 将前瓣向前翻转, 后瓣向后翻转, 分别与鼻腔外侧壁黏膜和钩突前方黏膜相对合(* 为切开 的泪囊) 。
表 1 80眼术后转归情况
眼数(%) 溢泪程度 正常 轻度 中度 重度 P 轻度(n=3) 2(66.7) 1(33.3) 0(0) 0(0) 中度(n=27) 24(88.9) 2(7.4) 1(3.7) 0(0) 0.021 重度(n=50) 37(74.0) 12(24.0) 0(0) 1(2.0) 表 2 不同泪道阻塞患者一期转归
眼数(%) 阻塞原因 眼数 治愈 有效 无效 外伤 7 5(71.4) 1(14.3) 1(14.3) 鼻部手术后 10 9(90.0) 1(10.0) 0(0) 放疗后 2 1(50.0) 1(50.0) 0(0) 原发性泪道阻塞 鼻中隔偏曲 14 11(78.6) 3(21.4) 0(0) 中鼻甲肥大 1 1(100.0) 0(0) 0(0) 慢性鼻窦炎 6 5(83.3) 1(16.7) 0(0) 慢性鼻窦炎伴鼻中隔偏曲 7 5(71.4) 2(28.6) 0(0) 正常或无需处理的鼻腔鼻窦病变及结构异常 33 26(78.8) 5(15.2) 2(6.1) -
[1] 周兵, 唐忻. 鼻内窥镜下鼻内泪囊鼻腔造孔术(附35例疗效分析)[J]. 耳鼻咽喉头颈外科, 1994, 1(2): 80-83. https://www.cnki.com.cn/Article/CJFDTOTAL-EBYT402.004.htm
[2] Wormald PJ. Endoscopic Sinus Surgery: Anatomy, Three Dimensional Reconstruction, and Surgical Technique[M]. 4th ed. Adelaide: Thieme, 2018: 161-176.
[3] 陈新军, 王向东, 王月, 等. 泪囊窝与毗邻结构解剖关系的CT影像学研究[J]. 中国耳鼻咽喉头颈外科, 2020, 27(2): 67-70. https://www.cnki.com.cn/Article/CJFDTOTAL-EBYT202002004.htm
[4] Alsulaiman N, Alsuhaibani AH. Bicanalicular Silicone Intubation for the Management of Punctal Stenosis and Obstruction in Patients With Allergic Conjunctivitis[J]. Ophthalmic Plast Reconstr Surg, 2019, 35(5): 451-455. doi: 10.1097/IOP.0000000000001315
[5] Cohen O, Amos I, Halperin D, et al. Five-and 10-Year Outcomes for Primary Endoscopic Dacryocystorhinostomy: Failure Rate and Risk Factors[J]. Laryngoscope, 2021, 131(1): 10-16. doi: 10.1002/lary.28528
[6] Cho K, Kim YD, Woo KI. Comparison of external and endoscopic dacryocystorhinostomy for distal canalicular or common canalicular obstruction: A retrospective study of 44 lacrimal systems[J]. Clin Otolaryngol, 2019, 44(4): 693-697. doi: 10.1111/coa.13358
[7] Allen KM, Berlin AJ, Levine HL. Intranasal endoscopic analysis of dacrocystorhinostomy failure[J]. Ophthalmic Plast Reconstr Surg, 1988, 4(3): 143-145. doi: 10.1097/00002341-198804030-00004
[8] Basmak H, Cakli H, Sahin A, et al. What is the role of partial middle turbinectomy in endocanalicular laser-assisted endonasal dacryocystorhinostomy?[J]. Am J Rhinol Allergy, 2011, 25(4): e160-165. doi: 10.2500/ajra.2011.25.3598
[9] Lee KC. Outcomes of posterior lacrimal sac approach in endoscopic dacryocystorhinostomy: review of 35 cases[J]. Am J Rhinol, 2008, 22(2): 210-213. doi: 10.2500/ajr.2008.22.3149
[10] Yang JW, Oh HN. Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy[J]. Graefes Arch Clin Exp Ophthalmol, 2012, 250(10): 1509-1513. doi: 10.1007/s00417-012-1992-x
[11] Movaghr M, Kodsi S. Merola C. Probing for nasolacrim al duct obstruction with intravenous protocol sedation[J]. J AAPOS, 2004, 11(3): 179-182.
[12] Maheshwari R. Success rate and cause of failure for late probing for congenital nasolacrimal duct obstruction[J]. J Pediatr Ophthalmol Strabismus, 2008, 45(3): 168-171. doi: 10.3928/01913913-20080501-17
[13] Cui YH, Zhang CY, Liu W, et al. Endoscopic dacryocystorhinostomy to treat congenital nasolacrimal canal dysplasia: a retrospective analysis in 40 children[J]. BMC Ophthalmol, 2019, 19(1): 244. doi: 10.1186/s12886-019-1256-1
[14] 王炳慧, 俞文哲, 季洁, 等. 复发的外伤性泪囊炎的治疗经验[J]. 临床耳鼻咽喉头颈外科杂志, 2014, 28(5): 341-342. https://www.cnki.com.cn/Article/CJFDTOTAL-LCEH201405026.htm
[15] Karpishchenko SA, Beldovskaya NY, Aleksandrov AN, et al. Experience in navigation system use in surgical treatment of the traumatic dacryocy stitis recurrence(clinical case)[J]. Ophthalmology J, 2019, 12(1): 83-88. doi: 10.17816/OV2019183-88
[16] Wormald PJ, Kew J, Van Hasselt A. Intranasal anatomy of the nasolacrimal sac in endoscopic dacryocystorhinostomy[J]. Otolaryngol Head Neck Surg, 2000, 123(3): 307-310. doi: 10.1067/mhn.2000.105416
[17] Uludag G, Yeniad B, Ceylan E, et al. Outcome comparison between transcanalicular and external dacryocystorhinostomy[J]. Int J Ophthalmol, 2015, 8(2): 353-357.
[18] Bothra N, Vasanthapuram VH, Ali MJ. Infantile Endoscopic Dacryocystorhinostomy: Indications, Anatomical Considerations, and Outcomes[J]. Ophthalmic Plast Reconstr Surg, 2020, 36(4): e100-e103. doi: 10.1097/IOP.0000000000001615
-




 下载:
下载:
