Analysis of prognostic factors for survival in patients with head and neck mucosal melanoma
-
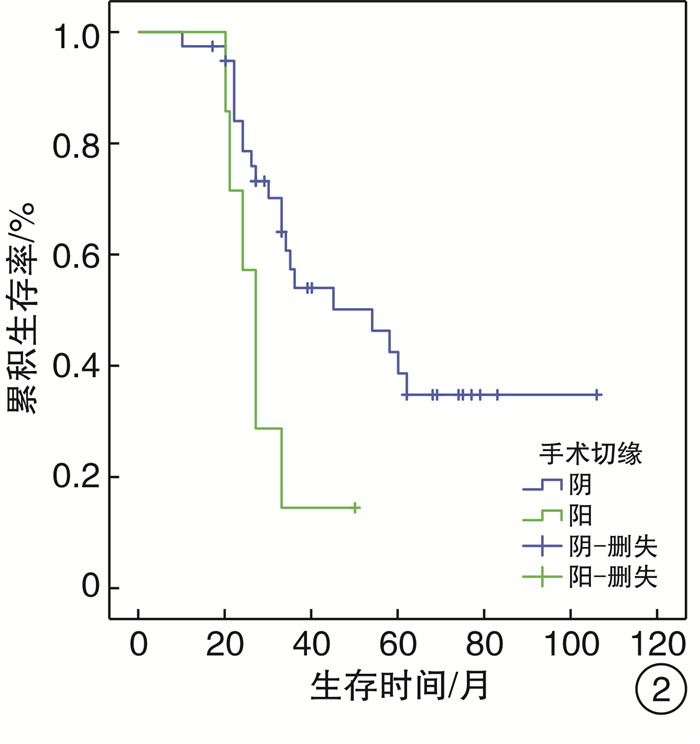
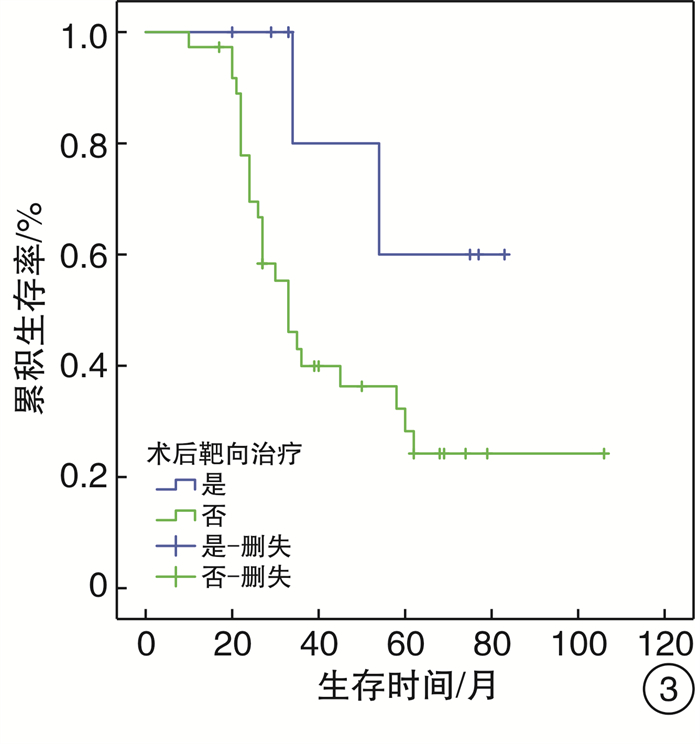
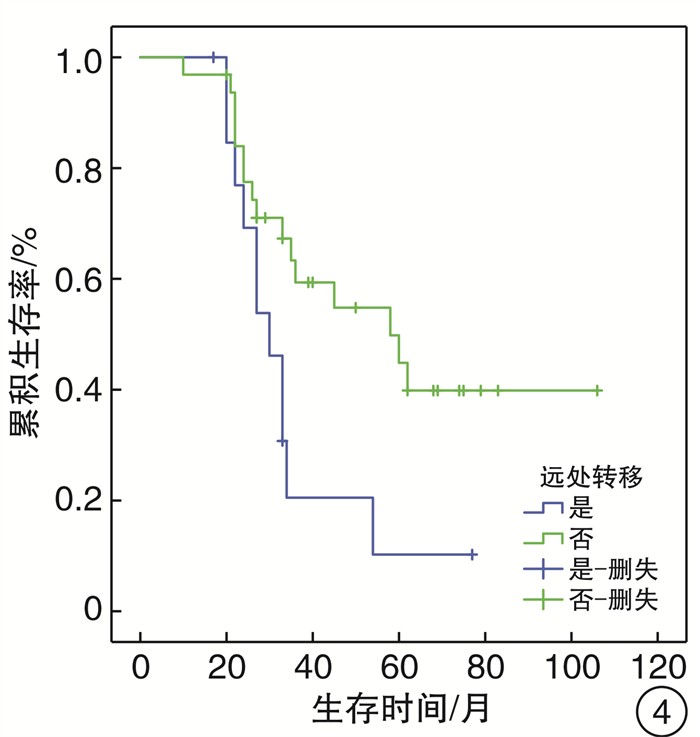
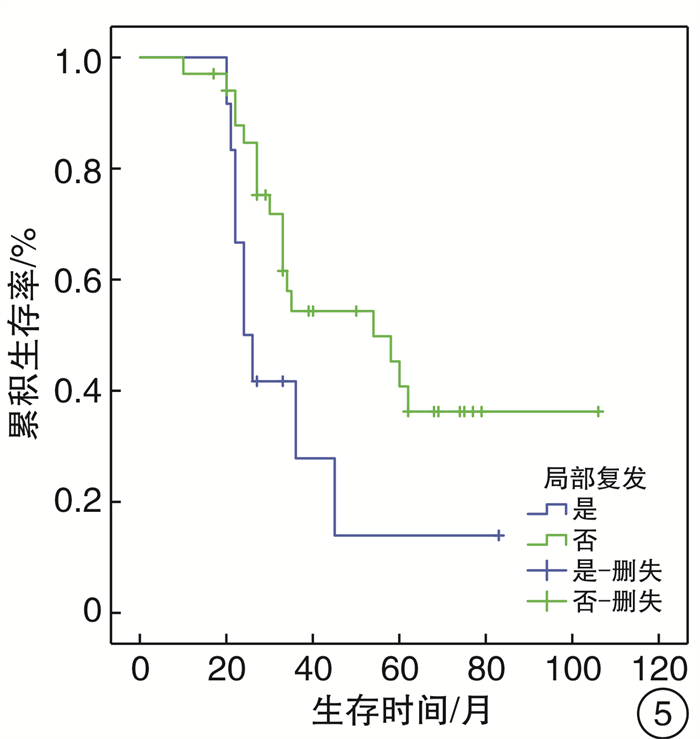
摘要: 目的 探讨头颈部黏膜恶性黑色素瘤(HNMM)的临床及病理特点, 手术治疗及辅助治疗对患者生存预后的影响。方法 回顾性分析46例HNMM患者的临床资料, 对影响患者生存预后的危险因素进行分析。生存分析采用Kaplan-Meier法, 单因素分析采用Log-rank检验, 多因素分析采用COX比例风险模型。结果 46例HNMM患者3年和5年的累积生存率分别为47.5%、34.1%, 中位生存时间36个月。单因素分析显示: 肿瘤分期、手术切缘、术后靶向治疗、术后远处转移、术后局部复发对HNMM患者生存预后的影响具有统计学意义(P < 0.05);多因素COX回归分析显示: 术后远处转移、肿瘤分期、手术切缘阳性是影响HNMM患者生存预后的独立危险因素, 术后应用靶向治疗是其保护性因素。结论 HNMM恶性程度高, 生存率低, 早期诊断、早期彻底手术切除是提高患者生存预后的首要方法, 术后辅助靶向治疗可能是改善患者生存预后的干预措施。Abstract: Objective To analysis the clinical and histopathological features, and the effect of surgical treatment and adjuvant therapy for the survival in patients of head and neck mucosal melanoma(HNMM).Method A retrospective analysis was conducted on the clinical data of 46 patients with HNMM, and the factors related to survival were analyzed. Kaplan-Meier analysis was used for survival analysis. Log-rank test was used for univariate analysis, and COX proportional hazard model was used for multivariate analysis.Result The 3 and 5 year cumulative survival rates of 46 patients with HNMM were 47.5% and 34.1%, respectively, and the median survival time was 36 months. Univariate analysis revealed that the factors affecting survival rates in patients with HNMM included tumor staging, surgical margins, postoperative targeted therapy, distant metastasis and local recurrence(P < 0.05). Multiple factor COX regression analysis showed that distant metastasis, tumor staging, surgical margins were independent risk factors for survival rates in patients with HNMM, and postoperative targeted therapy was the protective factor.Conclusion HNMM is of high malignancy and low survival rate. Early diagnosis and complete surgical resection are the primary methods to improve the survival, and postoperative targeted therapy may be an intervention to improve the survival.
-
Key words:
- head and neck neoplasms /
- mucosal melanoma /
- prognosis /
- survival analysis
-

-
表 1 影响HNMM患者生存预后的单因素分析
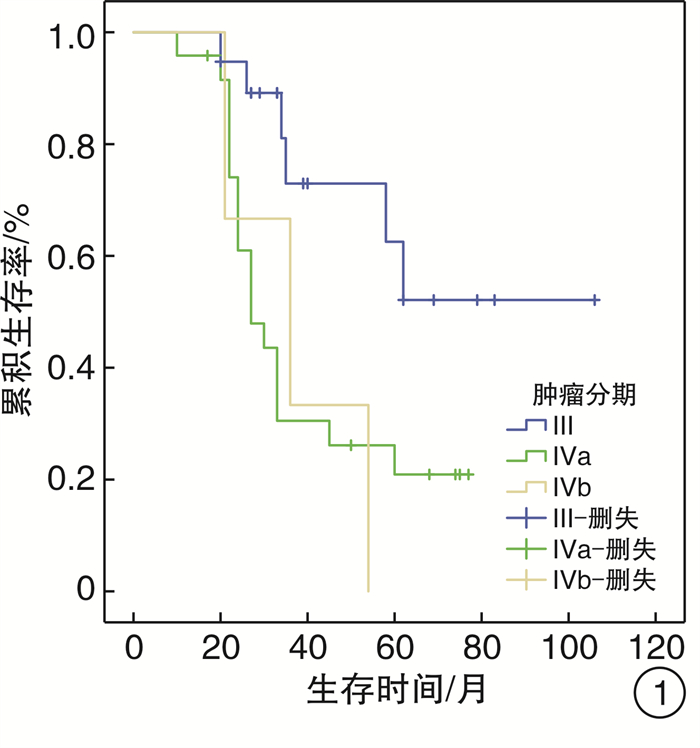
临床特征 例数 累积生存率 χ2 P 临床特征 例数 累积生存率 χ2 P 3年 5年 3年 5年 年龄/岁 1.853 0.173 手术次数 0.308 0.579 ≥60 22 9(40.9) 6(27.3) 1 38 17(44.7) 13(34.2) < 60 24 13(54.2) 9(37.5) 2 8 2(25.0) 2(25.0) 性别 0.053 0.818 手术方式 0.516 0.473 男 26 11(42.3) 8(30.8) 开放手术 39 28(71.8) 19(48.7) 女 20 11(55.0) 8(40.0) 内镜手术 7 5(71.4) 2(28.6) 发病部位 1.179 0.882 手术切缘 5.452 0.020 鼻窦 23 9(39.1) 7(30.4) 阴 39 21(53.8) 15(38.5) 鼻咽部 7 5(71.4) 3(42.9) 阳 7 1(14.3) 1(14.3) 鼻中隔 4 2(50.0) 2(50.0) 术后放疗 0.247 0.619 口腔 5 3(60.0) 1(20.0) 是 20 7(35.0) 6(30.0) 口咽及喉部 7 4(57.1) 4(57.1) 否 26 15(57.7) 10(38.5) 色素类型 0.721 0.396 术后靶向治疗 4.206 0.040 有 33 17(51.5) 14(42.4) 是 9 7(77.8) 5(55.6) 无 13 5(38.5) 2(15.4) 否 37 15(40.5) 10(27.0) 瘤细胞形态 2.036 0.565 术后局部复发 4.230 0.040 上皮样细胞 28 13(46.4) 12(42.9) 是 12 3(25.0) 2(16.7) 梭形细胞 7 3(42.9) 1(14.3) 否 34 18(52.9) 14(41.2) 杆状细胞 4 3(75.0) 0(0) 术后淋巴结转移 0.104 0.747 未分化细胞 7 4(57.1) 1(14.3) 是 3 2(66.7) 1(33.3) 肿瘤分期 8.196 0.017 否 43 20(46.5) 15(34.9) Ⅲ 19 14(73.7) 12(62.2) 术后远处转移 5.392 0.020 Ⅳa 24 7(29.2) 5(20.8) 是 14 3(21.4) 1(7.1) Ⅳb 3 1(33.3) 0(0) 否 32 19(59.4) 14(43.8) 表 2 影响HNMM患者生存预后的COX多因素分析
因素 B Wald值 RR 95%CI P 远处转移 1.514 8.107 4.545 1.603~12.886 0.004 肿瘤分期 - 7.004 - - 0.030 手术切缘 1.303 6.491 3.680 1.351~10.025 0.011 术后靶向治疗 -2.013 6.026 0.134 0.027~0.666 0.014 -
[1] 郭伟, 尹高菲, 陈晓红, 等. 头颈黏膜恶性黑色素瘤远处转移特点及相关因素分析[J]. 临床耳鼻咽喉头颈外科杂志, 2018, 32(14): 1078-1081. https://www.cnki.com.cn/Article/CJFDTOTAL-LCEH201814009.htm
[2] Wu Y, Wang L, Ma X, et al. The existence of early stage oral mucosal melanoma: A 10-year retrospective analysis of 170 patients in a single institute[J]. Oral Oncol, 2018, 87(3): 70-76.
[3] 连斌, 郑楠, 迟志宏, 等. 232例晚期黏膜黑色素瘤患者的一二线治疗疗效及预后影响因素[J]. 中国肿瘤生物治疗杂志, 2017, 24(3): 253-258. https://www.cnki.com.cn/Article/CJFDTOTAL-ZLSW201703010.htm
[4] Tyrrell H, Payne M. Combatting mucosal melanoma: recent advances and future perspectives[J]. Melanoma Manag, 2018, 5(3): MMT11. doi: 10.2217/mmt-2018-0003
[5] Maeda T, Yoshino K, Nagai K, et al. Efficacy of nivolumab monotherapy against acral lentiginous melanoma and mucosal melanoma in Asian patients[J]. Br J Dermatol, 2019, 180(5): 1230-1231. doi: 10.1111/bjd.17434
[6] Altieri L, Eguchi M, Peng DH, et al. Predictors of mucosal melanoma survival in a population-based setting[J]. J Am Acad Dermatol, 2019, 81(1): 136-142. doi: 10.1016/j.jaad.2018.09.054
[7] 孙士然, 易俊林, 髙黎, 等. 头颈部黏膜恶性黑色素瘤手术联合放疗的预后分析[J]. 中华放射肿瘤学杂志, 2018, 27(12): 1041-1045. doi: 10.3760/cma.j.issn.1004-4221.2018.12.002
[8] Jethanamest D, Vila PM, Sikora AG, et al. Predictors of survival in mucosal melanoma of the head and neck[J]. Ann Surg Oncol, 2011, 18(10): 2748-2756. doi: 10.1245/s10434-011-1685-4
[9] 刘志萍, 王凯, 黄晓东, 等. 52例原发鼻腔鼻窦黏膜恶性黑色素瘤疗效分析[J]. 中华放射肿瘤学杂志, 2016, 25(4): 327-331. doi: 10.3760/cma.j.issn.1004-4221.2016.04.006
[10] Lundberg M, Haapaniemi A, Hagstrom J, et al. Similar survival outcome after endoscopic and open approaches for sinonasal mucosal melanoma[J]. Rhinology, 2019, 57(2): 132-138.
[11] 尹高菲, 郭伟, 陈晓红, 等. 头颈部黏膜黑色素瘤117例临床特点及预后分析[J]. 中华耳鼻咽喉头颈外科杂志, 2018, 53(9): 668-674. doi: 10.3760/cma.j.issn.1673-0860.2018.09.006
[12] Schaefer T, Satzger I, Gutzmer R. Clinics, prognosis and new therapeutic options in patients with mucosal melanoma: A retrospective analysis of 75 patients[J]. Medicine(Baltimore), 2017, 96(1): e5753.
[13] 孙士然, 易俊林. 头颈部黏膜恶性黑色素瘤的临床诊治现状及进展[J]. 中华放射肿瘤学杂志, 2017, 26(4): 466-469. doi: 10.3760/cma.j.issn.1004-4221.2017.04.022
[14] 于雅莲, 李巍. 鼻及鼻窦黏膜黑色素瘤患者临床资料回顾性研究[J]. 现代肿瘤医学, 2018, 26(6): 853-856. doi: 10.3969/j.issn.1672-4992.2018.06.009
[15] Samstein RM, Carvajal RD, Postow MA, et al. Localized sinonasal mucosal melanoma: Outcomes and associations with stage, radiotherapy, and positron emission tomography response[J]. Head Neck, 2016, 38(9): 1310-1317. doi: 10.1002/hed.24435
[16] Yamashita C, Otsuka A, Nomura M, et al. Successful treatment of metastatic mucosal melanoma with a Del579 c-KIT mutation by imatinib after treatment of anti-PD-1 antibody[J]. J Eur Acad Dermatol Venereol, 2019, 33(3): e92-e93.
[17] Guo J, Si L, Kong Y, et al. Phase Ⅱ, open-label, single-arm trial of imatinib mesylate in patients with metastatic melanoma harboring c-Kit mutation or amplification[J]. J Clin Oncol, 2011, 29(21): 2904-2909. doi: 10.1200/JCO.2010.33.9275
-




 下载:
下载: